

Back to Public Benefit Corporation main page
|
Columns DCWatch
Archives Elections Government and People Budget issues Organizations |
FUTURE VISION: THE URBAN HEALTH CAMPUS ON
CAPITOL HILL District of Columbia Health & Hospitals Public Benefit Corporation February 2001PBC2:Urban Health Campus on Capitol HillNew Medical Campus Includes Mental Health, Long-Term Acute Care, Substance Abuse Services, Federal/D.C. PartnershipNew Urban Health Medical CenterModern Hospital to Replace D.C. General Hospital In 2 Years; Strategic Partnership with Howard University Hospital and College of MedicineNPCC & PBC Clinics to Join ForcesPBC's Community Health Centers to Partner With Non-Profit Clinic Consortium to Focus on Primary Care, 330 Status, Much Greater AccessSchool Health: Focus on YouthNurses in District Public Schools, Including Charter Schools, to Emphasize Health Education, Preventive Medicine, Immunizations, ScreeningsPractice Plan for PBC PhysiciansPhysicians Will Organize Into a Corporation For the Purpose of Delivering Specialty CareThis presentation outlines a revised plan for the future of D.C. Health 8 Hospitals Public Benefit Corporation (PBC), to be implemented starting immediately. REVISED February 22, 2001 PBC2 Urban Health Campus
|
| Cause of Death | United States | District of Columbia |
| Heart Disease | 268.2 | 291.1 |
| Cancer | 200.3 | 258.1 |
| HIV/AIDS | 5.0 | 47.0 |
| Pneumonia and Influenza | 34.0 | 43.8 |
| Diabetes | 24.0 | 37.3 |
Source: Centers for Disease Control. Monthly Vital Statistics Report.
Vol. 45, No 11(s)2, June 12, 1997:64-65
While the reasons for the District's high death rates are multi-faceted and complex, a large proportion of deaths from medical causes occurs prematurely and may have been prevented altogether. An analysis of adult inpatient deaths during 1998 at D.C. General illustrates how some of Washington's poorest people die. For patients over 65 (n = 153), the most common cause of death was sepsis (20.9%), frequently secondary to untreated diabetic wounds. Cancer was the most common cause of death among patients ages 45 to 64, accounting for 28.3% of deaths (n = 120). For patients 45 and under, AIDS accounted for 49.1 % of deaths (n = 114).
The leading causes of death among the uninsured residents of the District are from largely preventable causes and can be effectively managed in the ambulatory setting. Heart disease, cancer and hypertension, which disproportionately plague African Americans, are largely caused, and therefore complications can be controlled, by modifying risk factors. The spread of HIV could be virtually eliminated if high-risk behaviors were eradicated. Emergency rooms and hospitals bear the brunt of the current system's failure to promote health and prevent preventable disease. The top diagnoses of the uninsured who present at D.C.'s hospitals, presented in Table 11 bear this out:
Table II. Percent of Uninsured by Admitting Diagnosis*
| Admitting Diagnosis | Percent Uninsured |
| Trauma to the skin, subcutaneous tissue and breast age greater than 17 | 39.36% |
| Alcohol/Drug Dependence Detoxification and Rehabilitation | 26.72 |
| Poisoning and Toxic Effects of Drugs | 26.61 |
| Alcohol/Drug Abuse or Dependence, Detoxification or other treatment | 20.56 |
| Disorders of the pancreas except malignancy | 18.03 |
| HIV with major related condition | 14.64 |
| Cellulitis, age greater than 17 | 16.61 |
| Diabetes | 11.12 |
| Pneumonia and pleurisy | 9.99 |
| Chest pain | 9.98 |
| Psychosis | 4.75 |
| Heart failure and shock | 4.15 |
Source: Providing a Safety Net: District Hospitals Caring for the Uninsured. Washington, DC: DC Hospital Association, undated.
As the table indicates, the ill effects of poor access to mental health and substance abuse services is equally troubling to the uninsured. A recent report estimated there were 76,000 people with a substance addiction in the District, with only 12.5 percent admitted to treatment facilities (Wong, 1997). It is not surprising, then, that DC ranks highest in the nation, when compared to the state both the number of emergency room visits per thousand population and the number of hospital admissions for drug or alcohol abuse.
While the data present a bleak picture of the health status of the District's uninsured, they also paint a clear picture of the direction the city's health system must take to improve health disparities and, ultimately, the quality of life for the District's most vulnerable residents. That direction is the PBC2.
Like the PBC, PBC2 will offer the full continuum of primary, specialty and tertiary care. This care is driven by a profound knowledge of the consumers the PBC serves--D.C.'s medically unserved and underserved residents, traditionally presenting at medical institutions with advanced, multi-system disease and a host of related social issues. The PBC 2 will encompass the PBC's six community health centers and the 13 members of the Non-Profit Clinic Consortium and incorporate substance treatment services, mental health, and long-term care into this expanded existing care continuum. It will implement a number of new systems of administrative and clinical accountability in the areas of utilization management, performance improvement, disease management, and financial management. It will be headquartered at the existing historical site of DC General Hospital, which will be transformed into a new Urban Health Campus on Capitol Hill. Like the current PBC, it will continue to serve the-needs of all patients seeking care at its facilities, including families and childless adults, regardless of ability to pay.
In the process of looking to the future, the Council of the District of Columbia through the leadership of Council Members David Catania, Sandy Allen and Kevin Chavous have put on the table a methodology for looking at development of a fully integrated health care delivery system with headquarters on the grounds of D.C. General Hospital, which dates to 1806 and has been located at the same site (under many names) since the 1840s. An integral part of the Urban Health Campus will be a new Federal/District Partnership that will involve organizations such as the National Institutes of Health, Howard University Hospital and the Howard College of Medicine, and the Non-Profit Clinic Consortium (NPCC) in the design and operation of the Urban Health Campus.
These partnerships will allow the District an opportunity to utilize broad expertise in healthcare management and NIH research capabilities while also affording NIH a setting to continue research and training. Many of NIH's institutes and centers could locate facilities on the campus, such as the National Institute of Diabetes and Digestive and Kidney Diseases, National Institute on Aging, National Institute on Drug Abuse and National Cancer Institute. Campus-based healthcare services will collaborate with our partners in these programs.
To replace D.C. General Hospital, the PBC2 will build a modem medical center on the existing campus, ideally located at the intersection of 19th Street and Independence Avenue, S.E., immediately adjacent to the existing Metro subway station. The hospital will be built in 1 '/2-to-2 years at a cost of $100 million to $130 million, to facilitate creation of a cost-efficient healthcare delivery center. Transition costs over the two years will be $130-$150 million. However, PBC Chief Executive Officer Michael Barch is "confident" that the $150 million estimate is over-stated because it holds revenues and expenses constant. He fully anticipates that revenues will be increased by a minimum of $800,000 a month over the transition period while costs will be reduced significantly.
The new Urban Health Campus Medical Center will operate 190 beds with an anticipated daily average of 160 occupied beds, compared with D.C. General's current 250-bed staffed facility and 165 average current occupancy. The new hospital could feature a strategic partnership with Howard University Hospital and Howard's College of Medicine, to provide a range of services, which will result in economic efficiencies.
Included in the new Urban Health Campus Medical Center will be a Level I Trauma Center, Emergency Room and Urgent Care Center, to continue the historic role in treating patients from neighborhoods in Southeast and Northeast Washington; a Women's Health Center, with a modern birthing facility; a Senior Wellness Center to serve the District's aging population, and many of the inpatient and outpatient services currently offered at D.C. General. Working with our strategic partners - NIH, Howard and the non-profit clinics- we will focus our services on disease-specific institutes and primary care.
In order to assure desired health outcomes, integration of the IDS will occur on two levels: (1) the micro level (i.e., between providers and service) and, (2) the macro level (i.e., between population health statistics, trends and system design). Features essential to achieve complete integration include:
The installation of an integrated information management system allows micro level integration through:
At the macro level system reports will allow trends to be identified and disease management programs designed to educate PCP's, and to treat and educate patients.
Specialty referrals and services for enrolled patients will only be available upon referral from the PCP. Results of specialty services will be forwarded to the PCP after each visit/procedure.
The school health program will be integrated into the IDS utilizing the Department of Pediatrics as an expert resource available to School Health for programmatic initiatives. In addition, each school nurse will be pared with a pediatrician within the IDS network to serve as a resource when questions arise.
The PBC2 will deliver the following health care services:
1. Community-Based Primary Care Services
The PBC2 will offer community based primary care services at least six Community Health Centers, presently located in Wards Two, Six, Seven and Eight, and at the 28 historical safety net clinics that are members of the Nonprofit Clinic Consortium. This integrated system of primary care offers experienced patient care teams that can immediately provide culturally appropriate clinical and social support services in the city's neighborhoods that are home to its medically at-risk residents. Most importantly, because the PBC2 partner organizations represent the city's historical safety net providers, the PBC2 offers patients the continuity of ongoing relationships with clinicians who know them and their health histories. It is this continuity of relationships that will help the PBC2 to effectively manage and be accountable for the health needs of the target population.
2. Inpatient Hospital Service
The PBC2 will assure continuity of care and access to care for the city's most vulnerable residents of Wards 5, 6 and 7 by maintaining inpatient hospital services at D.C. General Hospital. D.C. General Hospital is a teaching hospital (with programs for interns and residents from Howard University and Georgetown University) and is fully accredited by the JCAHO and licensed by the District of Columbia. NPCC providers will apply for admitting privileges at D.C. General Hospital and will be able to admit patients, follow them during acute care episodes and participate in discharge planning.
D.C. General Hospital will house five inpatient care units
General Surgery/Trauma (22N/S, 23S)
Intensive Care, Adult (SICU, MICU, CCU)
Internal Medicine and Oncology (43 N, 52 N/S)
Maternal/Child Health (Labor and Delivery, OB2, Nursery, Peds, NICU)
Post Anesthesia Care Unit
Particularly noteworthy is the inclusion of ICU beds, which are lacking in the District of Columbia, in spite of apparent over-bedding. (At this writing, the 20 ICU beds at DC General Hospital are occupied, with four patients waiting in the ER for beds.)
3. Ambulatory Care Clinics
The D.C.. General Campus also houses primary care clinics offering adult medicine, pediatrics and well-woman care.
Specialty clinics on the campus include: An In/Out Surgery Clinic and a Diagnostic Center (where endoscopy, esophagoscopy, bronchoscopy, sigmoidoscopy, percutaneous endoscopic gastrostomy, colonoscopy, and liver biopsy are performed.) Medical subspecialty clinics such as Allergy, Asthma, Cardiac/Pacemaker, Gastrointestinal, Hematology, Hypertension, Oncology, Pulmonary, Renal, Rheumatology, Sarcoid and ENT, Neurology, Neurosurgery, Ophthalmology, Orthopedics, Podiatry, Liver, Thoracic/Vascular, Urology and Audiology clinics, an ob/gyn suite, a Cardiac Catheterization Lab, a Dialysis unit, an EEG Laboratory and a Physical Medicine and Rehabilitation unit.
All specialty, diagnostic and acute services available at the D.C. General facility are available to the target population of uninsured patients. The Medical Director may authorize appropriate services outside of the network on a case-by-case basis. Post specialty care, all patients will be referred back to their PCP for follow up. Necessary, ongoing specialty care will be performed in consultation with and on referral from the PCP.
4. Emergency Care Center
The Emergency Care Center (ECC) will continue to provide 24-hour access to major medical, major trauma, urgent and minor medical and minor trauma services. The institution operates as a Level I Trauma Center and the busiest Emergency Department in the city. The ECC is point of entry for 70-80% of the hospital's admissions and will provide 24/7 back up for the PBC2's community-based primary care physicians. It is anticipated that the number of ECC-originated hospital admissions will decline as the systems for preventive care mature. Triage and registration processes will be EMTALA compliant. Patients will be discharged for follow up with their PCP, as identified by the PBC2 electronic enrollment system and a copy of the treatment record will be faxed to the PCP for the patient's medical record. Uninsured patients presenting without a PCP will be assigned to and referred back for follow up to a PCP in geographic proximity to their home.
5. Dentistry and Oral Surgery
The PBC2 will offer dental services to adult and pediatric inpatients and outpatients on the D.C. General Campus and in community-based settings. Dental and oral surgery care includes:
- Comprehensive General Dentistry to medically compromised patients with special needs and patients referred for oral health problems
- Diagnostic, preventive and therapeutic periodontal services
- Comprehensive pediatric dental services for all children
- Ambulatory adult and pediatric anesthesia during complex dental procedures
- Maxillofacial prosthodontics for patients requiring oral facial reconstruction and prosthesis
- Endodontic services necessary to support the restorative treatment of patients
- Comprehensive dental services for oncology patients
6. School Health Program
The PBC2 brings a dedicated team of school health nurses and school health leaders to assure that mandated health services in the D.C. Public and Charter schools are culturally relevant, timely and designed to promote physical and emotional well being.
Once health screening identifies the need for further assessment and/or treatment, children without PCPs are referred to the nearest health center for further management. Multidisciplinary meetings between the health center staff and the school nurse staff enhance the integration of services of the neighborhood health centers and the School Health program.
7. Centers of Excellence
The PBC2 is planning to establish two centers of excellence. The diseases to be managed under the Center of Excellence model are selected based on the demographics of the population, top morbidity and mortality data for the city and the top acute care diagnoses for the uninsured.
The Diabetes Management Center will provide culturally relevant dietary assessment and planning, ophthalmologic assessments and renal protective therapy. The Center for HIV/AIDS Management will offer outreach and state-of-the art therapies to support optimal functioning and well being of individuals diagnosed with HIV/AIDS.
Both centers will adopt the disease management model, treating patients across a continuum of care through medication, specialized protocols and case management. Regular preventive care, beginning early in the disease process, and patient empowerment through education will be cornerstones of the Centers, with these goals:
- Improve functional status
- Reduce morbidity and premature mortality
- Control costs through effective disease management
- Acquire more meaningful outcomes data
- Improve ability to bear financial risk for services
- Improve patient and physician satisfaction
To eliminate process bottlenecks and other patient barriers at the outset, Center-based programs will incorporate patients into design through both qualitative and quantitative data gathering. Future plans are being formulated to establish a Center for Preventive Cardiovascular Disease, including comprehensive assessment and management of risk factors and a Center for Chronic Pulmonary Disease Management.
8. Pharmacy
Effective clinical management of the chronic diseases which drive the District's third-world-like morbidity and mortality rates demands access to appropriate, cost-effective pharmaceuticals delivered under a comprehensive clinical management plan. Indeed, patients with hypertension and diabetes require pharmaceuticals for control and prevention of tertiary complications. The PBC2 will continue to have DOD purchasing power, so that pharmacy expense can be maintained at the current PBC level of $2.1 million for the extant PBC sites and increased only marginally for other sites.
9. Mental Health, Substance Abuse and Long-Term Care Services
In keeping with the Urban Health Campus and PBC2 concepts, we have held preliminary talks with MedLINK Hospital at Capitol Hill, and District behavioral health leaders, about immediate action to establish new services on the D.C. General Hospital campus - services that will result in a new revenue stream immediately and continue during the transition period. Existing facilities will be used immediately and these services will become part of the new, integrated medical campus (see attached proposals).
MedLINK Hospital will locate 60 long-term acute care beds and up to 160 nursing home beds in existing D.C. General space as soon as Spring of 2001. MedLINK later will occupy 100 or more beds in the new hospital (the 100 beds are in addition to the 190-bed general hospital facility). In addition to leasing space, MedLINK will contract for services from D.C. General, such as radiology, meals, laboratory, pharmacy and housekeeping. Overall, this will generate new revenues to the PBC exceeding $14 million.
Separately, the PBC has received a behavioral health proposal to transfer 100 to 115 acute care psychiatric beds from St. Elizabeth's Hospital, operated by the Commission on Mental Health Services. The majority of these beds are for individuals committed for the first 72 hours as a "danger to self and/or others." Sixty percent of these inpatient admissions are also dually diagnosed, with mental health and addiction problems, at least half of whom are in immediate need of concurrent services. The District currently receives no Medicaid reimbursement for this acute inpatient care (rules do not allow reimbursement for a free standing mental health unit not connected to a general hospital), which costs $14.6 million a year to the District Government. But, by locating in D.C. General and the new Urban Health Campus Medical Center, potential Medicaid reimbursement for inpatient psychiatric beds will be about $22.8 million a year.
Between the two programs referenced above, it is estimated that new annual revenues of $26 million a year net will flow to the PBC2/UHC.
In addition, PBC2 providers will coordinate with the Commission on Mental Health Services and APRA to assure coordinated care for patients with behavioral health histories, including the dually diagnosed. To assure access to substance abuse services, including detoxification services for members of the target population, the PBC2 will negotiate an expansion to this contract to maintain a substance abuse unit on the D.C. General campus. The unit will offer Level IV services as defined by the American Society of Addiction Medicine (ASAM) in a therapeutic environment offering an organized, interdisciplinary and culturally competent program of detoxification and substance abuse management, including transition to residential and/or aftercare settings, for patients that, at some stage in their recovery or due to dual diagnosis, require an acute care setting.
10. Correctional Health Care
The PBC2 will continue to meet the acute and nonacute medical and dental needs of the city's incarcerated or custodial populations under a negotiated reimbursement agreement. Under such a contract the PBC2 will coordinate and collaborate to assure the provision of safe, accessible, quality and culturally relevant services
11. Other Health Programs
The PBC2 will coordinate and cooperate with the Department of Health to assure that (a) PBC2 patients are enrolled in outcome enhancing programs; and, (b) the city's funded Title V activities are optimally available to and used by women and children. The PBC2 expresses its willingness to negotiate mutually agreeable contracts with the Department of Health to assure ongoing operation of any related maternal and child program services.
12. Medical Education Program = Medical Excellence
The PBC2 will continue the PBC's role of providing graduate medical education programs with medical students from Georgetown and Howard universities, because these students improve overall performance and create an atmosphere of learning that enhances patient care. Howard University will resume its OB/GYN residency program which was discontinued five years ago and discussions will take place with George Washington University Medical School on resuming residency programs, as well.
The PBC2 and UHC will bring several new efficiencies and a transformed governance structure to bear on the fiscal feasibility, quality and accountability of the safety net health care delivery system.
The PBC2 shall establish a system-wide Performance Improvement Plan (PIP) to assure effective management of resources, provision of exceptional service and achievement of optimal health outcomes for patients. Through a written PIP, the PBC2 will remain focused and accountable to a planned, systematic, collaborative, network- wide approach to planning, measuring, assessing and improving the performance of the PBC2.
The Board of Directors delegates oversight (but not accountability) for performance improvement monitoring to a PI Committee whose members are geographically representative of the practitioner network, including primary care physicians and specialists in high-volume specialties. Practitioners represent no more than two-thirds of the membership, which also includes care and utilization management professionals, patient services and administrative representatives. The Committee is chaired by the Medical Director, who leads the members through the review and evaluation of policies, programs and utilization and recommends action to the CEO and the Board of Directors. The Committee assures allocation of resources for organization-wide projects and technical assistance to all structured performance improvement activities as needed.
The scope of the Performance improvement Program includes
Annually, the PI Committee will identify at least one clinically relevant issue for in-depth analysis and improvement. For years one and two, the PI studies will facilitate implementation of the Centers of Excellence Programs.
The clinical information system, managed under the scope of the PIP will provide data to enable the PBC2 to establish baseline measures and follow clinical indicators over time. These indicators will be relevant to the target population, providing meaningful data to help the PBC2 achieve its goal to reduce health disparities, particularly with respect to diseases managed through the Centers for Excellence. To measure both outcomes and the effectiveness of processes, such as access to care, across the network, PBC2 will produce nationally standardized HEDIS measures designated for the Medicare and Medicaid population. These include
The PBC2 shall utilize the SMS INVISION application for the capture of patient demographic, financial and clinical information, including PCP assignment. The SMS INVISION system will also be used to schedule patient encounters and capture service charges. Additionally, the 3M CODE 3 medical record abstracting and coding system, Digimedics Pharmacy system, Softmed Transcription and Chart Tracking application, SMS OPENLab and SMS Radiology systems will be utilized to support the clinical and regulatory requirements of the organization and the contract.
The PBC2 shall utilize the claim data to report patterns of use, costs and service utilization according to periodic and ad hoc timeframes. The PBC2's data systems will help support performance improvement activities, including utilization management and physician profiles.
The physician provider practice (PPP) will be formed by the medical and dental staff of D.C. Health and Hospitals Public Benefit Corporation (PBC) to provide financial incentives to assure that the programmatic and financial objectives of the medical and dental staff are congruent with and complement the objectives of PBC2. This arrangement will assure that accountability for the costs and outcomes of care, including patient satisfaction, is shared. The physician provider practice offers a full complement of medical, surgical and dental subspecialists with decades of shared experience in caring for the special needs of the uninsured population across a continuum of care settings.
Facilitating the operational efficiency and effectiveness of the PBC2 will be the consolidation of existing employment rules, regulations and bylaws into a single, comprehensive set. This consolidation will benefit both labor and management by making the administration of union rules less complex and time-consuming.
The makeup of the PBC Board of Directors will be changed to provide for designated representation by such partners as labor, the PBC Medical/Dental Staff, the Non-Profit Clinic Consortium, and the community which will require legislative action by the Council of the District of Columbia. In addition, a new procedure will be established for the nomination and selection of individuals to serve on the Board. The PBC Board Nominating Committee will develop lists of candidates from the community at large, including those with healthcare and business experience, and those with wealth. For each vacancy, the Nominating Committee will submit three names to the Mayor and Council for their final selection of one person.
To carry out the vision of PBC2, a management team has been assembled under the leadership of current PBC CEO Michael M. Barch, a long-time health care leader who has focused on the health care needs of the uninsured. His long and distinguished career has taken him from a position as Chief Executive Officer of George Washington University Medical Center, founder of Healthcare for the Homeless, HealthRight and an executive at Johns Hopkins.
Joining Mr. Barch on the management team is Robin Newton, M.D., the Chief Medical Officer of the PBC, who has devoted her entire medical career to caring for vulnerable populations at DC General Hospital. An internist by training, Dr. Newton has shaped the evolution of the continuing medical education programs, the Phoenix Center for patients with HIV/AIDS, and has practiced in both the acute and primary care sides of the delivery system. Other experienced operations, financial and clinical staff will be drawn from the existing PBC, as well as external sources.
The PBC2 vision does not permit continued operation of D.C. General Hospital in its current space, because the old facility is inefficient and drains scarce District financial resources. Facilities costs alone are running between $10 million and $15 million a year. A new hospital could be capitalized from the savings of not having to operate a white elephant.
Financial projections, including the cost of the new hospital and transition costs, are attached to this proposal. Also included are the cost of retaining a Level I Trauma Center on the DC General Hospital site, a pharmacy program for the uninsured, and funding of many "hidden" costs of operating a safety net for the unserved and underserved, including the uncompensated cost of care for inmates of the DC Department of Corrections and patients brought to the emergency room by Youth Services, St. Elizabeth's Hospital, the Metropolitan Police Department, the Metropolitan Area Transit Authority, the US Marshall, and other local and federal agencies.
Included on the revenue side of the equation are the savings to be effected beginning in May of 2001 from recent reductions in force at the PBC and revenue improvements expected from current efforts to bring the PBC's charges into alignment with the local marketplace.
In addition, the District Government Chief Financial Officer and the DCFRA have both mandated that the PBC do everything possible to optimize reimbursement rates. This will be accomplished through increased charges, bringing PBC rates closer to citywide hospital average charges. Medicare rates, for example, must be increased by at least 25 percent to avoid a complex Medicare reimbursement process that has penalized the PBC because its stated charges are actually lower than costs.
The increase also will help with Medicaid reimbursement and will be applicable for the balance of the current fiscal year, bringing in an estimated $21.6 million of additional revenues not currently budgeted and bringing overall PBC expenses and revenues close to breakeven in the coming months.
Legislation also will be proposed to ensure that the PBC 2 Proposal can work, by providing the PBC with guaranteed financial independence to operate separate from District Government regulations governing procurement, personnel and financial management. The PBC also will seek full independent banking and bonding authority, as was included in the original PBC Act of 1996.
The focus of the PBC2 is on patients and patient care, with a plan that must address every aspect of that focus. Our mission and vision is to create a modern community hospital as part of an integrated medical campus. The PBC must live within its allocated budget, earn anticipated revenues, operate efficiently, and address the medical needs of District residents to the greatest possible extent - regardless of any individual's ability to pay for services.
We have a unique opportunity to take advantage of emerging collaborative arrangements today to begin implementation immediately. In so doing, the PBC and District Government can meet requirements of the Federal Government that a fiscally sound plan for the future is put in place.
A public private partnership could provide a potential capitalization mechanism for construction of a new hospital and Urban Health Campus facility, which will strengthen the financial position of the District.
The financial model included in this proposal was derived from an analysis of the current cost of care for both insured and uninsured residents in the District of Columbia, pieced together from an in-depth review of the financial documents furnished to all RFP bidders by the Financial Authority, and productivity indicators based on "best models," with baselines established in reports from the Cambio consultants to the Financial Authority.
Further, the financial projections assume that the PBC2 would be reimbursed according to the current Medicaid regulations, i.e. Medicaid outpatients and DSH payments (federal funds forwarded to providers who take care. of a large number of indigent patients) would not be considered as part of the city's subsidy to the PBC. Further, it is assumed that the School Health Program would be fully funded at $8.4 million. We also have included a cost-of-living wage increase for all PBC employees.
The following financial model is conservative, and doable! It does not reflect significant new revenues expected to start in FY2001, as a result of the Financial Authority/District CFO mandate to increase PBC charges - resulting in an estimated $21.6 million of new revenues for balance of the current year, with increased Medicare and Medicaid reimbursement (See above).
| Hospital | Community Health Centers | Speciality Clinics | School Health Program | Total | |
| Revenues | |||||
| Patient Care | $64,051,000 | $2,624,968 | $5,500,000 | $0 | $72,754,268 |
| Local share of DSH & OP visits | $2,400,000 | $335,000 | $600,000 | $0 | $3,335,000 |
| DC Payment | $30,868,367 | $13,344,000 | $0 | $1,612,004 | $45,824,371 |
| Other | $1,982,400 | $0 | $495,600 | $0 | $2,478,000 |
| Special DC Payment | $7,184,744 | $5,549,733 | $15,851,780 | $1,438,871 | $30,025,128 |
| Subtotal | $106,486,511 | $21,853,701 | $22,447,380 | $3,050,875 | $153,838,467 |
| Intra-District Revenue | |||||
| DOC | $6,400,000 | $0 | $0 | $0 | $6,400,000 |
| MCH | $0 | $0 | $0 | $0 | $0 |
| HIV | $0 | $0 | $900,000 | $0 | $900,000 |
| SNP | $0 | $0 | $0 | $4,400,000 | $4,400,000 |
| SHP | $0 | $0 | $0 | $954,000 | $954,000 |
| WIC | $0 | $571,000 | $0 | $0 | $571,000 |
| Steam | $1,198,000 | $0 | $0 | $0 | $1,198,000 |
| Others | $272,000 | $0 | $0 | $0 | $272,000 |
| Subtotal Intra-District Revenue | $7,870,000 | $571,500 | $900,000 | $5,354,000 | $14,695,500 |
| RIF amount to be reimbursed | $2,190,728 | $0 | $547,682 | $0 | $2,738,410 |
| Total Revenues | $116,547,239 | $22,425,201 | $23,895,062 | $8,404,875 | $171,272,377 |
| Expenses | |||||
| Regular | $121,703,114 | $25,690,388 | $26,340,304 | $6,088,194 | $179,822,000 |
| RIF Savings & adjustments | ($8,030,968) | ($3,265,187) | ($2,445,242) | $2,316,681 | ($11,424,716) |
| Wage Adj (cost of living incr) | $2,875,093 | $2,875,093 | |||
| Subtotal | $116,547,239 | $22,425,201 | $23,895,062 | $8,404,875 | $171,272,377 |
| Revenue over (under) Expenses | $0 | $0 | $0 | $0 | $0 |
| Hospital | Community Health Centers | Speciality Clinics | School Health Program | Total | |
| Revenues | |||||
| Patient Care | $64,051,000 | $1,508,071 | $8,000,000 | $0 | $73,559,071 |
| Local share of DSH & OP visits | $2,400,000 | $225,000 | $800,000 | $0 | $3,425,000 |
| DC Payment | $41,661,699 | $14,844,000 | $14,699,462 | $3,050,875 | $74,256,036 |
| Other | $1,982,400 | $0 | $495,600 | $0 | $2,478,000 |
| Subtotal | $110,095,099 | $16,577,071 | $23,995,062 | $3,050,875 | $153,718,107 |
| Intra-District Revenue | |||||
| DOC | $6,400,000 | $0 | $0 | $0 | $6,400,000 |
| MCH | $0 | $0 | $0 | $0 | $0 |
| HIV | $0 | $0 | $900,000 | $0 | $900,000 |
| SNP | $0 | $0 | $0 | $4,400,000 | $4,400,000 |
| SHP | $0 | $0 | $0 | $954,000 | $954,000 |
| WIC | $0 | $571,500 | $0 | $0 | $571,500 |
| Steam | $599,000 | $0 | $0 | $0 | $599,000 |
| Others | $272,000 | $0 | $0 | $0 | $272,000 |
| Subtotal Intra-District Revenue | $7,271,000 | $571,500 | $900,000 | $5,354,000 | $14,096,500 |
| Total Revenues | $117,366,099 | $17,148,571 | $24,895,062 | $8,404,875 | $167,814,607 |
| Expenses | |||||
| Regular | $115,356,692 | $16,875,468 | $24,895,062 | $8,404,875 | $165,532,097 |
| Expense adjustments | $0 | $0 | $0 | $0 | $0 |
| Wage Adj (cost of living incr) | $2,282,510 | $0 | $0 | $0 | $2,282,510 |
| Subtotal | $117,639,202 | $17,148,571 | $24,895,062 | $8,404,875 | $167,814,607 |
| Revenue over (under) Expenses | $0 | $0 | $0 | $0 | $0 |
| Clinic | Ward | Street Address | Patients | Visits | Organizational Budget | Total Staff |
| Columbia Road Health Services | 1 | 1660 Columbia Road, NW | 1,896 | 7,208 | $1,300,000 | 30 |
| Community Medical Care | 2 | 1118 9th Street, NW | $428,232 | 10 | ||
| Community of Hope Health Center | 1 | 1417 Belmont Street, NW | 4,300 | 18 | ||
| Family and Medical Counseling Services | 6 | 2041 MLK Jr. Ave. SE | 2,472 | 3,814 | $1,800,000 | 41 |
| La Clinica del Pueblo | 1 | 1470 Irving Street, NW | $1,784,998 | 30 | ||
| Mary's Center for Maternal & Child Care | 1 | 2333 Ontario Road NW | 3,240 | 33,104 | 43 | |
| Planned Parenthood | 2 & 7 | 2 locations | 9,750 | 9,747 | 27 | |
| So Others Might Eat | 2 | 60 O Street, NW | 3,444 | 6,389 | 25 | |
| Spanish Catholic Center | 1 | 1618 Monroe Street, NW | 2,389 | 17 | ||
| Unity Health Care | 1-8 | 14 locations | 26,008 | 101,767 | $7,800,000 | 209 |
| Washington Free Clinic | 1 | 1525 Newton Street, NW | $870,000 | 145 | ||
| Whitman Walker | 2 & 8 | 2 locations | 1,373 | 14,773 | $6,000,000 | 33 |
| Zacchaeus Free Clinic | 2 | 1525 7th Street, NW | 1,550 | 6,852 | $1,700,000 | 58 |
| Total | 49,733 | 190,343 | $35,683,230 | 686 |

Unity Health Care, Inc.
Washington, D.C.
formerly Health Cure for the Homeless Project, Inc.
November 14, 2000
Mr. Michael Barch
Interim CEO
D.C. Health and Hospitals
Public Benefit Corporation
1900 Massachusetts Ave., S.E.
Washington, D.C. 20003
Dear Mr. Barch:
We have received your proposal regarding a possible collaboration between Unity Health Care, Inc. ("Unity's and the Public Benefit Corporation's ("PBC's") with respect to the primary care clinics and would like to express our support for the concept put forth in your proposal.
While there are still many important details to be negotiated, the idea of integrating the District's safety-net primary care clinics is intriguing and exciting. This merger is a logical next step for the District's primary care system and could result in significant cost-efficiencies and better health care outcomes for the District of Columbia uninsured residents. In addition, we strongly believe that Unity has a great deal to offer to such a collaboration, such as our clinical expertise and experience with this patient population, not to mention the benefits that accrue to recipients of Section 330 funds.
We look forward to hearing from you regarding our next steps.
Sincerely,
Vincent A. Keane
Executive Director
OFFICE OF THE EXECUTIVE DIRECTOR
3020 14th Street, N.W., Suite 401. Washington. DC 20009 202-518-6409 - fax: 202-462-6128
MedLINK HOSPITAL at CAPITOL HILL
700 Constitution Avenue, NE, Washington, DC 20002
Tel: 202.546.5700 Fax: 202.675.0411
November 9, 2000
Michael Barch, CEO
District of Columbia General Hospital
1900 Massachusetts Ave.
Washington, DC 20003
Dear Mr. Barch:
Please consider this request to relocate the operations of at least 60 long-term acute care (LTAC) beds and up to 160 nursing home beds to the DC General campus as soon as approved. Upon preliminary approval of this request, we would jointly conduct a comprehensive final proposal mutually acceptable before proceeding with the project.
MedLINK is the only LTAC operating in the District with a CON for 60 beds, expandable to 125. Typically, LTAC's are located within a hospital for mutual benefit. This is an especially good opportunity for DC General to offer additional services while reducing its cost of overhead.
The initial lease period requested is for 10 years with two additional 5-year renewal periods. MedLINK would pay the reasonable cost of renovating the space as needed. MedLINK would refer diagnostic testing and inpatient admissions to DC General.
In addition to leasing the space, the LTAC 8 Nursing Center will also need to enter into purchased service agreements with DC General for specific services. They are as follows:
The Largest benefit to DC General relates to the reduction of resource utilization in the Hospital due to the transfer of the long length of stay patients to the LTAC and Nursing Center.
The economic benefit to DC General from this project is preliminarily estimated to be $ 14,285,000.
Tables summarizing these benefits are attached for discussion purposes. Utilizing the hospital's latest Medicare Cost Report we can determine the prudent cost of the space we propose to lease and the prudent markup of services we would purchase to fully comply with Medicare law.
Thank you for allowing us to make this request. Thank you for the constant referrals of your hard to place long length of stay patients to MedLINK We are committed to provide the highest quality of care to your patients. It is our sincere desire to improve integration of services at DC General as well as improve its cash flow.
Respectfully Submitted,
Peter Shin, DPM
President
Attachments
| Benefit to DC General Hospital from leasing to a 60 bed LTAC | Annual Benefit (Estimated) |
| Space Lease for 60 beds (estimated at $5,000/bed) | $300,000 |
| Purchased Services from DC General (estimated at $75/patient day for 60 patients) | 1,642,500 |
| Drugs purchased from DC General | 1,080,000 |
| Medical House Coverage 24 hours daily | 100,000 |
| DC General Medicare DRG cost savings from Length of Stay reduction from LTAC being in-house (estimated at 5 patients daily costing $1,500/patient day)* | 2,737,500 |
| Additional short term acute care admissions to DC General by LTAC referral (10 referrals/month at $5,000 each)** | 600,000 |
| Lab, Radiology and other Diagnostic Services purchased from DC General | 500,000 |
| Total Potential Benefit | $6,960,000 |
* The largest benefit relates to the reduction of resource utilization
in the Hospital due to the transfer of the long length of stay patients to the LTAC.
**Although this may not be a true saving, it may create a situation in which capacity is
created to accept incremental admissions while minimally increasing variable costs.
Prepared by: Patricia D Hawkins, Ph.D.
Member, Systems/Model Work Group
DC General Hospital Transition Task Force
November 1, 2000
The potential closing/downsizing of DC General Hospital has generated a great deal of concern on the part of consumers, community health care providers, and DC General staff. Several task forces have been working on various hospital models (110 -140, 165 beds as well as a short term 23 hour community access hospital) but none have included an inpatient behavioral health component. We are proposing that whatever hospital model is eventually adopted that at least 100 behavioral health beds be included.
The proposed expansion of DC General to include a behavioral health unit is in keeping with the current plan of the Commission on Mental Health Services to close existing services at St. Elizabeths, build a new hospital at St Elizabeths to handle current Forensic and Geriatric cases, and transfer some 100 to 115 acute care psychiatric beds to a community general hospital. The majority of these l00 beds (60%) are for individuals committed for the first ?2 hours as a "danger to self and/or others " Sixty percent (60%) of these inpatient admissions arc also dually diagnosed, with mental health and addiction problems, at least half of whom (30%) are in immediate need of concurrent services. Most of these patients suffer from chronic mental illness, experiencing multiple hospitalizations, and many are homeless or near homeless with limited community support systems. On average, 50% of these admissions stay for more than 30 days, not because of their mental status but for lack of community resources These individuals present complex and unique challenges and need very specialized, culturally sensitive cage, a highly experienced staff, and extensive wrap-around services to secure and maintain entitlement benefits, housing, and long term support in the community.
The Commission on Mental Health Services is also in the process of implementing a CARE Point Initiative which will require designated care agencies to provide the full continuum of care, including acute hospitalization, under a case rate capitation. Such a system would require fee for service payment contracts for hospital services at St. Elizabeths or at a community general hospital. Needless to say, the ability to offset actual inpatient costs with Medicaid reimbursement will virtually guarantee that all Medicaid eligibles will be placed in community hospitals, rather than at St. Elizabeths.
In addition, CMHS has also developed a comprehensive Medicaid Rehab Opting scheduled for implementation in April 2001, which will provide Medicaid reimbursement for a more extensive list of community-based outpatient services All three of these Commission plans, transfer of acute care beds to the community, the Care Point initiative, and implementation of the Medicaid Rehab option, could provide the funds necessary to fully support a new, state-of-the-art acute care mental health unit of 100 beds or more associated with DC General.
Establish a minimum of 100 inpatient acute care beds in new state-of-the-art hospital providing involuntary commitment beds, acute care stabilization services, detoxification,. intensive substance abuse treatment services for the singly- and dually diagnosed, partial hospital services for patients in need, a step-down (non-acute care unit) for clients still in need of some Structure while awaiting benefits, housing, community treatment programs, etc. This unit would be pan of a new inpatient hospital and new outpatient service complex on the ground of DC General Hospital.
To provide a truly innovative service system, we are proposing the following. the addition of a 100 to 200 bed long term care facility (which is desperately needed in the District and would benefit from close proximity to mental health and addiction treatment services), the development of outpatient PPC primary care, CMHS mental health, and emergency from visits, promote the long term stability of the safety net, and improve the health status and health outcomes of District residents. Truly, this would be a national state-of-the-art model of an integrated community-based health care system, appropriate for the Nation's Capitol and for the dawn of the 21st century.
Transition Process. In preparation for receiving St. Elizabeths 100 acute care beds in 1997, DC General vacated a unit which remains vacant today. During the construction of the new hospital facilities which will include the behavioral health unit, St. Elizabeths patients and staff' could be transferred into this unit within the transitional DC General hospital, providing immediate savings of $40,000 a day to the city or some prorated amount if the transfer is phased in. These monies could then be used for essential renovations of the proposed transitional behavioral health unit and for initial construction costs of the new unit, as well.
Advisory Committee: Appoint a select advisory committee representative of consumers, providers, NPCC, DCPCA, DC General, CMHS, APRA, key Federal staff and union officials to work together to collect data, review the literature, gather appropriate input, identify "state-of-the-art" treatment and management systems, funding models, staffing patterns, and facility designs, and develop, within 30 days, final recommendations for the new DC Health Campus to be constructed on the grounds of DC General. This committee could then function in monitoring the transition and implementation plans, ensuring that this complex process moves forward as rapidly and efficiently as possible and with the full support of all parties committed to the continued existence of DC General Hospital services and the expansion and improvement of the entire health care "safety net" in the District of Columbia.
District of Columbia Health and Hospitals
Public Benefit Corporation
PBC Administration
1900 Massachusetts Avenue, SE
Washington, DC 20003
(202) 675-7655
Fax: (202) 675-5650
TO: Michael Barch
Interim Chief Executive
FROM: Michael Young, M.D.
President, Medical & Dental Staff
SUBJECT: Provider Practice Plan
There have been several attempts to establish a practice plan in this organization, first as D.C. General Hospital, and then as the Public Benefits Corporation. A practice plan committee was established in October 1997 and met somewhat regularly until June 1999. Bylaws for a practice plan and a management outline were adopted. We were unable to substantively engage the finance section of this organization to speak to billings and collections and hence, were unable to realistically talk about base pay and incentives. Therefore, we did not progress to the point of discussion on compensation agreements. Attached are two compensation models that were to be discussed by the practice plan committee at a meeting that never occurred. The private practice plan committee is currently not functional in the PBC. The CMO is the chair of this committee and no meeting has been called since June 1999.
The Medical and Dental Staff has in the past, and currently, supports a practice plan concept. I am certain that it could be revitalized if a commitment to our future existence is assured.
November 9, 2000
CONFIDENTIAL
Mr. Michael Barch
Chief Executive Officer
D.C. Health & Hospitals
Public Benefit Corporation
1900 Massachusetts Ave., S.E.
Suite 1450
Washington, D.C. 20003
Re: Talking Points and Diagrams of Potential Capitalization of Construction for New Hospital Facility
Dear Mr. Barch:
This is to thank you for meeting with us yesterday to discuss the possibility of utilizing a public private partnership to deliver cue to the residents of the District of Columbia. As promised yesterday, we slave attached a talking points outline arid two diagrams of a potential capitalism mechanism for construction of a new hospital and urban medical campus facility four D.C. General. Please note, we believe that these types of public-private partnerships have bean dote bra: for example, the District entered into a similar traps action with Corrections Corporation of America (see attached article we found on the internet). We also believe that Los Angeles has utilized a similar partnership arrangement to deliver care to its residents, although we are endeavoring to obtain additional information on eactl of these projects.
While this Material is submitted on behalf of our client, please note that the attachments are intended for discussion purposes only. Nothing should be construed as an offer. At this stage all discussions are preliminary in nature. Further diligence and legal research would be necessary to ensure both the success of the operation and compliance with applicable laws.
We appreciate your bringing this discussion forward and your support for it. We look forward to the possibility of working with you to preserve and enhance medical services to the District's residents.
If you have any questions or concerns regarding the attached or any other matter, please do not hesitate to call either Ken Gordon at 202/326-1500 or me at 202/326-1585.
Sincerely,
Michael H. Cook
RKG (4): Talking Points Outline
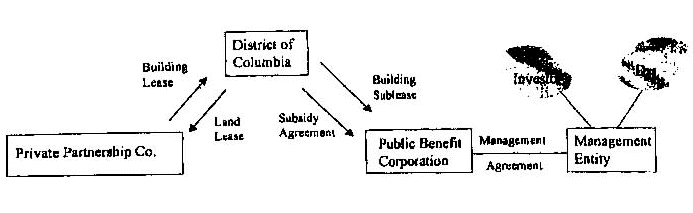
Diagram of Scenario A
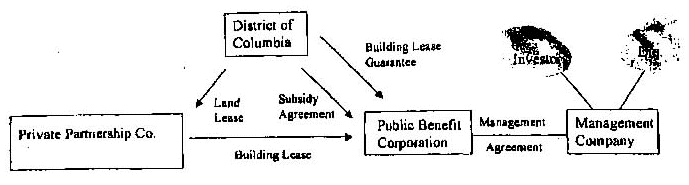
Diagram of Scenario B
Article from www.prnewswire.com
Cc: R Kenneth Gordon
CONFIDENTIAL
PRELIMINARY OUTLINE OF POTENTIAL CAPITALIZATION PLAN
FOR THE NEW D.C. GENERAL HOSPITAL
The following is a talking points outline of a plan for capitalizing a new hospital and health services facility for D.C. General Hospital. Through creation of a public-private partnership, the quality of health care services for residents of Washington, D.C., especially the medically indigent, can be enhanced. The financial position of the District could also improve.
Goals/Benefits
The Financing and Con Construction Plan. (See diagram attached.)
Operations. (Also, see diagrams attached.)
Caveat: This outline does not constitute an offer, and it is not binding on any patty. Significant research would be necessary to ensure compliance with all laws. Any actual proposal may vary significantly from the preliminary discussion.
Any questions should be directed to Michael H. Cook (202/326-1585) or R. Kenneth Gordon (202/326.1500) of Jenkens & Gilchrist. P.C.
1. The diagrams assume that the District or Public Benefits Corporation has m calf obtain an ownership or leasehold interest in the land that world enable it m least of sublease On land to Private Partnership Co. If that assumption is incorrect, the arrangement would be restructured to enable the lease of the land to Private Partnership Co.
Metropolitan Washington Council of Governments
February 1, 2001
Mr. Michael M. Barch
Chief Executive Officer
D.C. Health & hospitals
Public Benefit Corporation
1900 Massachusetts Ave.. S.E
Washington, D.C. 20003
Dear Mr. Barch:
I appreciate the opportunity to forward information on COG's energy performance contracting project. This project will be of particular interest to you because it can provide the means for the Public Benefit Corporation to make critical upgrades and replacements to infrastructure and facilities regardless of current budget constraints. You may be aware that COG has an agreement with Chevron Energy Solutions (CES) which makes customized, energy-related services and improvements available to various jurisdictions, agencies, and institutions throughout the Washington metropolitan area.
The Public Benefit Corporation was an initial principal to the UP that resulted in COG's agreement with Chevron Energy Solutions (see enclosures). Therefore, the Public Benefit Corporation can participate in the program simply by submitting a brief letter of request to Mr. Carl Kalish, Director of Contracts and Administrative Services. As you can see from the enclosed information (Energy Conservation Measures and Services Available under Contract). the range of services is quite extensive and could cover many of your capital improvement needs.
You may also know that energy performance contracting began as a method to rebuild aging, public sector, infrastructure at the local level. Now, however, private industry, the federal government, and especially the Department of Defense, utilize the process frequently and with a great deal of success. Building on past successful models, COG 's project has been designed to provide greater flexibility and potentially more benefits than most existing programs. Energy Performance Contracting, and particularly COG's: project, has a number of distinguishing features. For instance:
You may have been informed that CES representatives previously conducted a preliminary survey of your facilities and already have an idea of what type of savings can be achieved. In fact, an "authorization to proceed" agreement was in the process of being signed with the Public Benefit Corporation when the former CEO resigned. However, if after reviewing the enclosed information, you are prepared to sign such an agreement, please call me at your earliest convenience and 1 will have Chevron Energy Solutions forward the document to your attention.
Moreover, it is our understanding that overall plans for the retention and use of the entire building complex may have changed. Therefore, some conclusions derived for the previous survey results may no longer be applicable. Nonetheless, CES officials have informed me that they are confident that they can help you meet your facility upgrades and equipment replacement needs, despite funding shortfalls that may exist.
We would like the opportunity to meet with you and your staff in order to discuss this opportunity in more detail. We are available at your convenience. I can be reached at (202) 962-3387.
Sincerely,
Leo W. Young
Director, Special Projects
Enclosures
cc: Michael C. Rogers, COG Executive Director
Interior and Exterior Lighting Replacement and Control Improvements
Motor Replacement with High Efficiency Motors
Boiler Control Improvements
Packaged Air Conditioning Unit Replacement
Cooling Tower Retrofits
Economizer Installation
Facility Management System Replacement/Alteration
Computerized Management Control and Data Acquisition Systems (e.g., SCADA Systems)
Occupancy Sensors
LED Exit Sign Installation
Rewiring
Fans and Pump Replacement or Impeller Trimming
Chiller Retrofit/Replacement
Upgrade of natural Gas Fired Boilers with New Controls (Low Nox Burners)
Steam Trap Replacement and Maintenance
Insulation Installation
Variable Speed Drive Utilization
Window Replacement
Window Coverings and Awnings
Reflective Solar Window Tinting
Day Lighting Controls
Roof Replacement
Replacement and/or Conversion of Air Conditioning and Heating Units
Liquid Refrigerant Pump Addition to Reciprocating Air Conditioning Units
Refrigeration Equipment Replacement with High Efficiency Units
Transformer Replacement
Construction of New Co-generation Facilities
Solar Domestic Hot Water Systems
Solar Air Preheating Systems
Weatherization
Fuel Cell Installation
Fuel and Energy Procurement
Equipment Lubricants and Related Products
Petroleum Based Surface Coverings
Faucet Replacement (Infrared Sensors)
Water Efficient Bath and Kitchen Fixtures arid Accessories (Institutional)
Water Conservation System Installation
Water/Wastewater Treatment
Pumping Systems
Energy Rate Audits
Investment Grade Energy Audits
Engineering Services and Documentation
Project Financing and Related Financial Services
Training Services
Maintenance and Operations
Any other Measures that Enhance Energy and Water Consumption Efficiency, Improve
Operations, and Reduce Associated Energy Costs.
![]()
Send mail with questions or comments to webmaster@dcwatch.com
Web site copyright ©DCWatch (ISSN 1546-4296)