

Back to Public Benefits Corporation main page
|
Columns DCWatch
Archives Elections Government and People Budget issues Organizations |
TABLE OF CONTENTSCollaborating Organizations
Government of the DISTRICT OF COLUMBIAStrategies for ChangeHealth Care System Development CommissionFinal ReportMayor Anthony A. Williams, Chair December 2000 Strategies for ChangeFinal Report of the District of Columbia Health Care System Development Commission Ex-Officio Members Commission Members Staff Director Funding for the Commission provided by Technical consultation and research provided by the Economic and Social Research Institute Collaborating OrganizationsThe Economic and Social Research Institute (ESRI) (http://www.esresearch.org), based in Washington, D.C., is a nonprofit organization that conducts research and policy analysis in health care and in the reform of social services. ESRI specializes in studies aimed at enhancing the effectiveness of social programs, improving the way health care services are organized and delivered, and making quality health care accessible and affordable. The Robert Wood Johnson Foundation's State Coverage Initiatives program (http://statecoverage.net) helps states improve the availability and affordability of health insurance coverage, particularly for working families. Through providing states with grants, technical assistance, workshops, and information on best practices, the program is designed to build the policy making and technical capacity of states to address their unique health care coverage issues. The Robert Wood Johnson Foundation (http://www.rwjf.org), based in Princeton, N.J., is the nation's largest philanthropy devoted exclusively to health and health care. The Foundation concentrates its grantmaking in three goal areas: to assure that all Americans have access to basic health care at reasonable cost; to improve care and support for people with chronic health conditions; and to reduce the personal, social, and economic harm caused by substance abuse - tobacco, alcohol, and illicit drugs. The Academy for Health Services Research and Health Policy (http://www.academyhealth.org) provides a professional home and technical assistance resource for both researchers and policy professionals. Health services researchers and policy professionals benefit from increased communication and interaction, which help facilitate the translation of research into effective health policies. The Academy also helps researchers and policy professionals strengthen their skills and expertise through both technical assistance and expanded professional development opportunities (e.g., an annual meeting, health services research methods workshops, and other activities). The Academy aspires to be the preeminent source for stimulating the development, understanding, and use of the best available health services research and health policy information by public and private decision makers. About the CommissionMission and GoalsThe Health Care System Development Commission was established under the Health Care System Development Act of 1999. The Commission's goals were to identify strategies for: 1) Improving the overall health of District residents by building a health care delivery system that meets a full range of medical needs, irrespective of an individual's health insurance status or ability to pay for services; 2) Increasing access to care and individual choice through extending health coverage to a greater percentage of the District's uninsured; and 3) Building the Department of Health's capabilities to manage the health system and ensure public health. EXECUTIVE SUMMARYIn October 1999, Mayor Anthony Williams, together with Council Chair Linda Cropp and Human Services Committee Chair Sandra Allen, convened the Health Care System Development Commission to recommend strategies for transforming the District's health care delivery system into one that more effectively increases access to health services and emphasizes primary care (see Appendix A). The Commission submitted its recommendations in the form of a District Council Resolution in February 2000 (see Appendix B). These recommendations provide the District with a road map for better utilizing its public health dollars. More than $1 billion in public funds are spent annually on health care in the District. One overarching question is how to spend the money in a more cost-effective manner that will yield better health outcomes. To do this, the District should implement an integrated, phased-in set of changes in the health care system. This report analyzes possible new strategies, estimates their costs, and sets specific milestones and targets to improve outcomes. Depending upon the phase-in schedule, the District may require very limited new funding in the first years of implementing the recommendations. I. Improve the Health Care Delivery SystemBuild and Enhance its Network of Medical Homes. By establishing a health center certification process, the District could begin to strengthen its existing network of local public and private health centers that serve as the primary care, disease prevention, and health education providers for both large numbers of uninsured patients and Medicaid enrollees. In addition, the District needs to enhance the capacity of these health centers and increase funding for:
One mechanism for increasing funding is to raise Medicaid reimbursement rates to health centers that meet certain standards related to quality and efficiency and addressing unmet health care needs. By building the capacities of local health centers and enabling them to better provide primary care services, and maintaining a prescription drug program, the District can ensure that every resident - those with and without insurance - will have a "medical home" that is a stable source of primary and preventive care. Use New DSH Funds to Help Foster a Better Delivery System. The District should use new Disproportionate Share Hospital (DSH) payments and other public funding more effectively to develop and strengthen relationships between health centers and hospitals as well as other facilities, such as freestanding imaging centers, laboratories, ambulatory surgery centers, and specialty clinics. The District should develop an "Integrated Delivery System" whereby all levels of the health care system (from the community-based primary care providers to specialty centers and hospitals) work in tandem. Because the coordination of a full range of health care services is an important complement to building primary care capacity, each local health center needs to be part of a referral network through which it can lead patients to secondary and tertiary care. The District should move to purchasing specific services from cost-effective, high-quality public and private providers of indigent care. In this way, the District would become a more efficient purchaser of health care for both publicly insured and uninsured residents. This involves developing clear expectations about the cost and quality of the services it purchases. These expectations should be converted into standards that are built into requests for proposals (RFPs) and reflected in payments for services provided by managed care organizations, health centers, hospitals, and other providers. Establish Mechanisms for Funding Capital Improvement and Operational Needs. As a result of the constrained revenue streams that have traditionally supported primary care for the uninsured, many of the District's primary care facilities have unmet capital needs. Several are functioning in makeshift facilities and lack modern computer systems and other equipment. The District could help improve and expand the primary care system by developing a mechanism to aid public and private health centers in obtaining technical assistance and funds for capital improvements (including renovating facilities, purchasing equipment, and installing MIS). By aiding health centers in purchasing and renovating buildings in lower-income neighborhoods to serve as local medical homes, the city will also be taking a step toward stabilizing and improving these neighborhoods. These health centers also need assistance in serving uninsured patients, especially until a Medicaid expansion is fully implemented. This assistance can be achieved by enhancing Medicaid payments to centers, which will help offset the costs of providing care for uninsured individuals. In addition, the Commission proposes funding a program that will help individuals without prescription drug coverage receive necessary medications. II. Broaden Health Insurance CoverageExpand Medicaid Coverage. As enrollment initiatives proceed, the District should also begin a gradual expansion of DC Healthy Families (DCHF) coverage to low-income adults who do not presently qualify. Some of these individuals will become eligible if the District's current waiver application for a pilot DCHF expansion (to adults aged 50-64 without dependent children up to 50 percent of the federal poverty level (FPL)) is approved by the Health Care Financing Administration (HCFA). Each Medicaid expansion should be phased-in and evaluated midcourse so that we learn which strategies appear to work and which do not. A good next step is to cover all remaining adults with incomes up to 50 percent FPL and then proceed in stages to a threshold of 100 percent FPL. Full implementation of this process is envisioned to take between four and five years. Increase Private Sector (Employer) Coverage. The District needs to work with the private business sector through an initiative to make health coverage more affordable for both firms and workers. The District should begin this effort with a tax credit for employers to help cover a portion of the cost of health care premiums. This program would encourage employer-sponsored health insurance and, at the same time, help attract and retain businesses in the District. The Commission also recommends taking steps to assure that smaller firms have a broad and efficient purchasing pool available in order to make the cost of coverage affordable. Two options for creating a pool include: (1) "branding," in which people are grouped under a single title (e.g., those offered to D.C. government employees and Medicaid enrollees), with small businesses permitted to purchase coverage through this pool; and (2) gaining federal approval for District businesses to participate in the Federal Employees Health Benefits Program (FEHBP). Both of these options would allow small businesses to access health insurance at lower prices than are available in the general marketplace. III. Strengthen the Public Health InfrastructureBuild Health System Infrastructure. To develop and manage the changes outlined in this report, the District's Department of Health (DOH) needs to enhance its core public health capabilities. Central among these changes is the need for an integrated MIS capability, the development of baseline data, the completion of an updated and more effective State Health Plan, and a better integrated Certificate of Need (CON) process. In that regard, the Commission recommends that DOH:
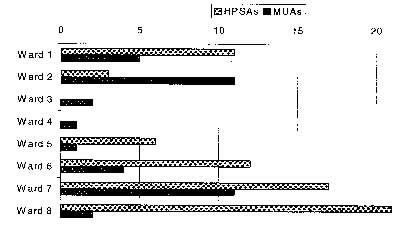
With these changes, the District will be better able to assess and further develop its health system and achieve real health improvements. IntroductionThe State of the District's HealthDespite the fact that an unusually large proportion of the District's population is enrolled in Medicaid (23 percent compared to a national average of 15 percent), an estimated 80,000 District residents remain uninsured (see Appendix C). However, the problem does not appear to stem from a lack of overall resources; public money allocated to health care for lower-income residents in the District alone totals more than $1 billion a year (see Appendix D). Furthermore, according to a 1997 report, the District's ratio of hospital beds and specialty physicians per 100,000 population were both more than two-and-one-half times the corresponding 1995 figures for the United States as a whole.1 The abundance of primary, hospital, and specialty care providers, however, are not equitably distributed throughout the city. Many neighborhoods of the District are underserved for primary and preventive health care (see Appendix E). Some 151 of Washington, D.C.'s 192 census tracts are designated by the federal Public Health Service as Primary Health Care Visit Shortage Areas, 36 are Medically Underserved Areas (MUAs), and 71 are Health Professional Shortage Areas (HPSAs). A report completed by the District's State Health Planning and Development Agency (SHPDA) noted that only 14.8 percent of all District physicians and 16.7 percent of primary care providers (PCPs) provide services in the 151 shortage areas. The lack of health insurance coverage and the uneven distribution of health care in the District mean that many lower-income residents face multiple barriers -including geography, lack of insurance, and cultural differences - in accessing primary and preventive care. In recent years, notable progress has been made in reducing some of the risk factors for poor health status. But the Commission recognizes the unusually high incidence of serious health conditions that continue to plague the District, including heart disease, cancer, tuberculosis, diabetes, and sexually transmitted diseases, all of which disproportionately affect lower-income individuals (see Appendix F). Many of these conditions may be avoidable if patients have access to timely health screening and preventive care. In other cases, diseases may be controlled if early diagnosis is followed by timely and appropriate treatment through medication, medical monitoring, further diagnostic tests, or surgery. The health care system must stress timely health care screening and early treatment, while also focusing on educating people about healthy lifestyle choices. This report outlines the recommendations of the Commission to change the current health care system to respond to the identified problems. The changes detailed in this report will require some additional costs. To help finance the cost of the proposals enumerated in this report, the District may draw upon or choose to reallocate portions of the following funds: EXHIBIT 1
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| Funding Categories | Amounts | ||
| Disproportionate Share Hospital (DSH) funds | $45.7 million1-1 | ||
| Federal | $32.0 million | ||
| District | $13.7 million | ||
| Tobacco settlement | $35.7 million1-2 | ||
| PBC direct subsidy | $44.4 million | ||
| MCH block grants | $3.6 million1-3 | ||
| Medical Charities | $0.7 million | ||
| TANF | $3.2 million1-4 | ||
| TOTAL | $133.3 million | ||
1-1 $12.9 million of this amount is from the
technical correction first allocated in FY2000; of this amount, $6.6 million is allocated
to the pilot Medicaid expansion program (not yet approved by HCFA).
1-2. Requires action by Executive and Council to determine spending.
1-3. Federal funds for women's and children's health only.
1-4. Federal funds for Medicaid outreach.
Note: Additional funds may emerge from Medicaid savings from managed care or reduced
fraud, but are not counted here. Savings may also be derived through the results of the
PBC management assessment and the resulting contracting for PBC services to the uninsured.
A critical element of the Commission's recommendations is the recommended steps to improve the health care delivery system. Improvements to the delivery system are a necessary primary step in a process that also includes phasing in a health insurance coverage expansion. This strategy has several key components.
District hospitals currently receive $45.7 million in DSH funding, including $12.9 million in new funding from a technical correction in FY 2000. As Medicaid expansion progresses, changes could be made in how the new DSH funds are distributed so that the hospitals can better assist the District in achieving its goal of a more integrated and efficient delivery system and are compensated in accordance with their proportionate share of indigent care (see Appendix G). In that regard, the Commission recommends that the District, to better connect DSH funds to community needs, adopt a process that includes three key components:
1. Match DSH funds (initially only new DSH funds) to community needs as closely as possible. Historically, the District has been unable to ensure this match is occurring. This reflects in part the use of other factors (e.g., services provided to Medicare and Medicaid patients) in DSH allocation formulas. To the extent possible, DSH funds should reflect the need for this care and the distribution of uncompensated care across the city. The Department of Health (DOH) should develop the capacity to track how District uncompensated care resources are spent, who received the services, and what results were achieved from these services. Uncompensated care costs should include only those services for which there is no source of even partial reimbursement. To receive DSH funds, hospitals should be required to code all diagnoses for uninsured patients.
2. Tie the receipt of at least a portion of these funds to a hospital's demonstrated commitment to form strong linkages between the primary care delivery system (including hospitals' own primary care clinics) and the services that are needed when primary care uncovers medical problems requiring further diagnosis and treatment. In the first year of this initiative, this might entail a hospital submitting a detailed plan to the District indicating how it intends to reach out to the primary care delivery system and form these relationships. In some cases, this integration is already in place. Examples include the PBC, whose network of health centers is integrated with DC General Hospital; Providence Hospital and Mary's Center; and Howard University Hospital and La Clinica del Pueblo.
Other requirements should involve providing the DOH with timely information on health care quality and outcomes.
| TARGET By no later than 2001, DOH, in consultation with District hospitals, should establish baseline data on: (1) the extent of emergency room use with a breakdown of how much of that use is inappropriate; and (2) the extent of ambulatory-sensitive-admissions (e.g., admissions for flare-ups of chronic conditions such as asthma and diabetes that should be preventable with timely preventive and primary care). This information, including details on the number of uninsured persons served and the, value of this care (based on diagnostic-related groups or other market measures), should be reported separately from data on services to District residents covered by Medicaid. Once a baseline is established, hospitals will be encouraged to decrease the number of inappropriate emergency room visits and the number of inpatient days resulting from delayed primary care by 20 percent.2 |
3. Develop long-term plans. In subsequent years, the District would expect to see specific steps taken to: (1) ensure that feeder systems are established between groups of health centers (including hospital primary care clinics) and hospitals; and (2) ensure that data on quality and outcomes are actually provided. The District should develop periodic reporting requirements for hospitals demonstrating the hospitals' progress toward these goals. Their compliance with these requirements and the information reported should be linked to the distribution of DSH payments.
In addition, a portion of the new DSH funds could be used to create a pool that would compensate hospitals for providing necessary diagnostic, outpatient, and inpatient services to persons referred from the health centers. This DSH fund would substantially augment the donated services that hospitals now provide through the Archdiocese Health Care Network in the District. Hospitals could be paid some proportion (e.g., 60 percent) of what other payers (e.g., Medicaid) might pay for these services. While these payments would be below the hospital's costs, these services would otherwise be provided without any compensation.
The basic idea behind this approach is to continue to provide DSH funds to the hospitals as long as the number of uninsured residents remains high, and to tie the receipt of these funds both to the distribution of the uncompensated care load and to the District's goal for a more integrated health delivery system in which all providers are held accountable-for both cost and quality. These requirements must be implemented in accordance with various federal rules requiring allowable uses of DSH funds.
An important part of the Commission's recommendations involves a series of measures to strengthen the District's health centers so that they can best serve lower-income residents. This will involve some support for capital needs, assistance with operating expenses, and help in improving MIS capacity.
Low-income District residents suffer from a lack of access to primary care. As a result, many individuals wait until late in the course of an illness to seek and receive care. This care is most frequently provided in hospital emergency rooms where treatment costs are high and outcomes can be far worse. The District's -health would benefit from a network of health centers that provide "medical homes" delivering critical and early primary care. These facilities would be located throughout the District, particularly in underserved neighborhoods, and would deliver quality care to both insured and uninsured individuals. The District can forge such a network by building on the capabilities of existing providers through capital investments, better use of Medicaid funds, and public-private partnerships.
The District has an existing network of public health centers affiliated with DC General Hospital and run by the PBC. In addition to the public health centers, the District has a group of primarily independent, private, not-for-profit health centers, and hospital-operated primary care centers that serve as medical homes for many lower-income people and high-risk groups, including the homeless, immigrants, children in poverty, and people with AIDS. According to data from the DC Primary Care Association, the PBC provides about one-third of all primary care visits to the uninsured in the District, and the private health centers handle the remaining two-thirds. The District, however, lacks a mechanism for certifying that its public and private health centers meet community-need related care accessibility and quality standards and a process for ensuring that these health centers are integrated within the larger health care safety net.
Through a certification process, the District could expand and coordinate its primary care and preventive services, reaching special populations not currently served by the public health system alone, and also help build supportive relationships with hospitals and other service providers. These relationships would ensure that the patients served by the health centers also receive the necessary diagnostic and specialty services they need.
To achieve this goal, the Commission recommends that the District establish a set of criteria by which all health centers could become District of Columbia Qualified Health Centers (DCQHCs). Certification under the DCQHC program would include technical assistance and the ability to receive increased reimbursement rates and capital funds. Criteria for DCQHCs need to be developed more fully in conjunction with the State Health Plan and CON law and should be established through a process that includes community input. These criteria may include:
| TARGET By the end of FY 2002, 18,000 to 20,000 uninsured District residents will have a local medical home (a DCQHC or health center with an approved plan to become a DCQHC) where they receive primary care, and through which they have access to comprehensive health care. |
Health centers with approved DCQHC plans would have access to technical assistance to help them gain full DCQHC status. The designation of DCQHCs is important as a first step in building a better primary care system. The DCQHC program would provide a way of monitoring the private-sector safety-net providers, with the goal of eventually having one set of criteria for all public and private safety-net health centers. This would provide a mechanism for making safety-net policy decisions inclusive of all public and private safety-net providers.
The DCQHC designation would allow the District to provide oversight for the activities of the providers it designates as DCQHCs. The city government could then require that the DCQHCs meet certain standards of service and quality, submit regular financial and performance reports, allow site visits, etc., as a condition of maintaining their DCQHC status. An additional advantage of the designation is that DCQHCs would become a component of the State Health and Medicaid State Health Plans and would be subject to DOH's CON approval process. In the absence of an official designation, planners must address each health center or provider as a unique entity.
Another way of building accountability into the system is to mandate that all health centers submit epidemiological data to the DOH. Health centers will be required to collect information about the health status of their communities and provide it to the DOH. This will enable them to allocate resources so that community health needs are recognized and met.
| TARGET By the end of FY 2002, at least 10 health centers will have approved plans to become DCQHCs. |
The District should establish a capital improvement fund to modernize and improve existing health centers (priority would be given to the public clinics), including their physical plants, equipment, computers, and MIS, as well as to build new health centers in underserved areas. The Commission recommends allocating this money to a public-private partnership, possibly under the aegis of the Local Initiatives Support Corporation (LISC), a private, non-profit organization that has worked for many years in community development. This partnership would develop linkages with banks, foundations, and corporations to provide technical assistance and funding (in the form of grants and loans) to non-profit organizations working in one of their service areas. LISC has already begun an initiative to assist local health and human service providers (see Appendix I). The District could subcontract, or award a competitive grant, for the administration of funds for capital development and technical assistance to LISC (or another community development organization) with a set of goals and guidelines. These funds would be earmarked for the health centers, and only DCQHCs or health centers with DOH-approved plans to become DCQHCs would be eligible to apply for the capital grants and loans. The administrative entity would manage the funds according to District guidelines and submit periodic progress reports to the District. These District guidelines would be developed using baseline data, the State Health Plan, and CON guidelines. Funds would be awarded to DCQHCs (and those with approved plans to become qualified) that are best able and willing to provide care in the most underserved areas in the District. By making some money available through loans rather than grants, the capital improvement fund could create a self-renewing pool of funds for community improvement.
The Commission proposes that $10 million be provided to this fund from District capital funds for use by PBC clinics and entities willing to contract with the city to operate clinics in District-owned buildings, such as unused parks and recreation buildings as well as purposely constructed new city-owned structures. A second portion of the investment fund may be supported by a one-time allocation of $5-15 million from the District's general fund or new funding sources which would be used to aid public/private health center partnerships and private health centers. Additionally, a portion of the cost could also be covered by some of the funding the District receives that is related to community development, such as the Community Development Block Grant. The funds allocated by the District could be matched by private-sector funds through LISC or a similar organization.
In addition to the need for the capital improvement fund described above, the Commission recommends that the DCQHCs (and those with approved plans to become DCQHCs) receive additional operational support payments to help offset the costs of providing large amounts of uncompensated care (at least as long as the District has a sizable number of uninsured individuals). The need for enhanced payment rates will decline as more of the District's population is covered by health insurance. The Commission's recommendation is to use enhanced Medicaid reimbursement rates to help DCQHCs that serve a very high percentage of uninsured patients in addition to their Medicaid population (see Appendix J).
The principle of recognizing that additional costs are inherent in caring for the historically medically underserved is already established in federal law, which mandates Medicaid reimbursement to the nationwide network of federally qualified health centers (FQHCs). By law (which may sunset in 2003), state Medicaid agencies now reimburse FQHCs based on their actual costs, in most cases paying the difference between Medicaid health plan rates and the FQHCs' costs. Some states, such as Maryland, have codified the principle, recognizing not only FQHCs, but also its own state network of Maryland Qualified Health Centers as eligible for cost-based reimbursement.
The Commission proposes establishing a similar reimbursement mechanism in the District whereby public and private health centers could apply to be certified as DCQHCs. DCQHCs that are certified or have DOH-approved plans to become certified will receive increased payments for the services they provide their Medicaid patients. These additional payments will help offset their costs for serving uninsured patients. The most advantageous way to do this is via augmented Medicaid payments, since it allows the District to claim the 70 percent federal match on payments made to these health centers. These augmented payments could most likely be made without obtaining a §1115 waiver from HCFA, because the District already negotiates payment rates with individual providers. By designating more health centers on behalf of Medicaid beneficiaries to receive higher Medicaid rates, more federal money would be brought into the city.
The purpose of a DCQHC augmented Medicaid program would be to provide, at least on a temporary basis, a baseline level of support for essential medical services that cannot be funded through other means. This model is another way the city can leverage its limited funds, since District Medicaid dollars going to DCQHCs would be matched by federal dollars as well as by the private dollars these health centers raise.
| TARGET By the end of FY 2002, three to four health centers will have begun receiving funds and technical assistance through the public-private partnership capital improvement fund. |
The Commission also recommends that the District continue the operation of the Pharmaceutical Drug Payment Assistance (PDPA) program that currently provides prescription medicines to uninsured persons. This program, which is currently funded with proceeds from a lawsuit against pharmaceutical manufacturers, will run out of funding in mid-2001. The estimated cost of maintaining this program is $2-3 million per year. Additionally, in order to maximize resources through this program, the District might seek to take advantage of the PBC's contract with the United States Department of Defense for purchasing pharmaceuticals.
The strategy to broaden health coverage in the District has two parts - expansions in Medicaid eligibility and financial incentives for employers to offer coverage.
In the past two years, the District has made significant strides in expanding Medicaid eligibility to populations previously not covered by Medicaid. The District has expanded eligibility to children up to 200 percent FPL via the State Children's Health Insurance Program (SCHIP) as authorized by the federal government's Balanced Budget Act of 1997 and parents of Medicaid- or SCHIP-eligible children via a nonwaiver expansion up to the same limit (see Appendix K). As these initiatives are relatively new, enrollment levels could be expanded. Program administrators expect lags in enrollment in the first 24 months of any expansion program, as newly eligible individuals become aware of their eligibility and educated about the program. Enrollment numbers for these expansion programs are slowly increasing as the District continues to expand its outreach efforts to these populations.
To further reduce the number of uninsured residents, the District has focused new expansion efforts on lower-income adults without dependent children, a population that makes up a large portion of the District's uninsured residents. In the Fall of 1999, the District submitted a waiver proposal to HCFA to expand Medicaid eligibility to adults without dependent children ages 50-64 with incomes under 50 percent FPL. Through this pilot program, the District anticipates enrolling roughly 1,200 adults at a total average annual cost of $6.6 million.
The Commission recommends expanding Medicaid eligibility to more of this adult population, beginning with individuals of all ages with incomes up to 50 percent FPL and expanding in phases over time to individuals of all ages with incomes up to 100 percent FPL. Expanding Medicaid eligibility to all adults without dependent children with incomes up to 100 percent FPL will render 14,000 additional individuals eligible for Medicaid. Using combined District and national participation and crowd-out rates, it is estimated that approximately 7,400 individuals will enroll by the end of year two of this five-year expansion effort (Exhibit 2). By the end of the five-year expansion, all adults without dependent children up to 100 percent FPL will be eligible for Medicaid. This includes more than 25,000 individuals. Roughly 15,000 of those eligible are expected ultimately to enroll, and an estimated 13,000 of this group would previously have been uninsured. The following table includes the enrollment and cost estimates for an incremental expansion initiative for adults without dependent children. Note that the enrollment and cost estimates for each phase of the expansion include those of the previous phase.
| Phase 1 | Phase II — Full Implementation by Year 4 or 5 | ||
| Year 1 | Year 2 | ||
| Income Level | 50% of poverty | 50% of poverty | 100% of poverty2-1 |
| Number Enrolled2-2 | 5,1842-3 | 7,411 | 15,000 (13,000 newly insured) |
| Total Cost | $14.2 million | $20.8 million | $41.8 million |
| Federal2-4 | $9.9 million | $14.6 million | $29.3 million |
| District | $4.3 million | $6.2 million | $12.5 million |
2-1. Enrollment and cost estimates for adults
without dependent children with incomes up to 100 percent FPL were determined using the
participation (or take-up) rates and crowd-out rates for those individuals with incomes up
to 50 percent FPL.
2-2. The Phase I I estimated enrollment numbers are annual averages for
a five-year waiver period, while figures for the 50 percent income level are monthly
averages in individual years (see Appendix L).
2-3. Includes pilot waiver population aged 50 to 64.
2-4. The federal share of the cost of the program must be budget neutral
to HCFA, meaning the amount of proposed federal spending under the waiver program cannot
exceed what federal spending would have been in the absence of the waiver program. To meet
budget neutrality requirements, the District can finance the federal share of the cost by
redirecting a portion of the existing federal Medicaid money (e.g., DSH payments) or
creating savings-from existing expenditures (e.g., enrolling Medicaid fee-for-service
beneficiaries into managed care arrangements) (see Appendix M).
The District has previously proposed several strategies for using some of its new DSH allotment to finance coverage expansion initiatives. The District currently receives a $32 million DSH allotment from the federal government and contributes matching DSH payments totaling $9.9 million to private hospitals.
One proposal is to expand DCHF coverage to adults without children. This would involve the District using the $9 million DSH adjustment (new DSH) to cover the federal share of the cost of enrolling newly eligible people in the first year. The District must use existing federal DSH dollars for this program to meet federal budget neutrality requirements. This would leave the original base $23 million DSH allotment untouched. This money would still be used to compensate hospitals in the District for providing care to large numbers of uninsured patients (see Appendix N).
Actual enrollment of the newly eligible adults might proceed more slowly than anticipated, as this population is very difficult to identify and enroll in Medicaid. Many of the adults without dependent children will have chronic medical conditions. Some are likely to have substance abuse problems. To better serve this population, as well as other adults and adolescents, the District should reassess the costs and benefits of adding substance abuse treatment as a covered service under Medicaid. As enrollment levels increase in Year 2 and the program is expanded to higher income levels in later phases, the District could consider using some of its remaining $23 million federal DSH allotment or generating savings from other parts of the Medicaid program to subsidize the cost of the program and meet budget neutrality requirements. If a future upward adjustment in federal DSH payments to the District is received (Congress is considering additional adjustments beyond $9 million), such funding could also be used to help finance the coverage expansion.
More than half of the people in the District without health insurance live in a household where someone is working. Thus, a key component to reducing the number of uninsured is to help lower-income workers obtain coverage by making it more affordable to their employers. The working uninsured are particularly prevalent among smaller firms. For example, only 55 percent of firms with between three and nine workers offered coverage nationwide, compared with more than 90 percent of firms with 50 or more employees.3 In addition, many small firms pay as much as 25 percent more for coverage than large companies. To address this problem, the Commission recommends that the District adopt two strategies.
The District should provide a tax credit to employers that would defray a significant portion of the health care premium. The Commission proposes a credit of $100 per month per employee that employers could claim against the cost of providing coverage for those workers who live in the District. To qualify for this credit, employers must contribute at least 50 percent of the premium cost of a standard insurance plan. This credit would represent about 25 percent of the average monthly cost of a standard plan for an employee and spouse, thus providing significant assistance to employers who offer coverage. If this tax incentive were offered for every covered DC resident employee, it would be prohibitively expensive and result in a relatively modest reduction of the uninsured for every dollar spent. For most large employers who already offer coverage, little additional coverage would be gained. To address this problem, the Commission recommends that the tax incentive be offered for the first five DC resident employees in each firm covered by a standard insurance plan for which the employer pays at least 50 percent. The advantage of this approach is that it would focus the tax incentive on firms with 10 employees and fewer, thus providing the best return for the District's investment, while not discriminating against larger employers. Another benefit of this recommendation is that it would make the District a more attractive place for employers and their employees, thereby contributing to the economic development of the city.
The District could strengthen coverage among small group employers by obtaining approval for them to participate in the Federal Employees Health Benefits Program (FEHBP). This approach has three important benefits: (1) it lowers the administrative costs for small employers, usually by at least 10 percent; (2) it would allow employees to choose from a broader range of plans instead of being limited to one or two plans; and (3) it would be relatively simple to implement and operate because much of the administrative infrastructure is already in place. The Commission believes that small businesses would significantly benefit from participating in FEHBP and recommends that the feasibility and mechanisms for exploring this alternative be further explored.
The Commission recommends that DOH improve its capacity to track and manage the District's health system and ensure the health of its residents. To strengthen the public health infrastructure, the District will need to fully implement a state-of-the-art outcomes measure-based MIS that links DOH to health care providers throughout the city and allows DOH to better track population health. It is also critical that the District's State Health Plan and State Medicaid Plan be written to serve as better tools in guiding the implementation of the health system improvements proposed by the Commission.. The Certificate of Need (CON) program should be restructured and regulations pertaining to provider reporting requirements should be reviewed to further assist the DOH in guiding reforms of the District's delivery system. The DOH should build its capacity to breathe life into the goals delineated by the Health Commission. This will involve redefining and evolving its CON program and State Health Plan into more effective tools for guiding health system development and the DCQHC program. The Department will need to establish a core data set of quality assessment measures for tracking and evaluating the entire health system and better targeting the expenditure of public dollars.
Improve outreach and enrollment capacity. The District should implement a computer and Internet-based enrollment process and expand outreach to enroll those already eligible for general Medicaid and DCHF. To date, the District, like most of the states, has fallen short of full enrollment in these programs, leaving a significant amount of federal matching money unused. An estimated 15,000 uninsured residents are eligible for one of these programs, but are not enrolled (see Appendix O). This represents approximately 19 percent of the uninsured. Maximizing federal dollars (TANF and SCHIP) available for outreach will require: (1) more and better-trained workers; (2) making greater use of "outplacement workers" (who are held accountable for enrollment rates) as allowed under federal Medicaid guidelines; and (3) a computerized, Internet-based enrollment system. The latter should function to allow hospitals and other providers to electronically submit applications to the city for eligibility and receive quick responses. Applicants can also receive online information about DCHF. This could help reduce the indigent care burden on hospitals and improve access to care for the uninsured by enrolling them into health plans that cover a wide range of preventive and primary care services. To succeed in this strategy, a new approach to enrollment must have four key components:
Irrespective of which option is chosen, an essential component of developing a seamless system of coverage for individual patients and populations is having an electronic system for the collection of aggregate data. All hospitals and community-based health centers should be capable of transmitting this data electronically to a central repository. This would facilitate a consistent base of information on cost and quality and encourage prompt payment of claims. All contracts with health providers serving vulnerable populations (including those providing mental health and substance abuse services), should contain a section on mandatory data reporting. Those data requirements should include basic encounter data as well as some subset of quality indicators.
| TARGET: By the end of FY 2002, DCHF computerized enrollment will be available in 50 percent of the District's hospitals and 20 percent of the District's community health centers (including hospitals' community-based primary care clinics). By the end of FY 2001, DOH will have implemented the first stage of a comprehensive MIS and prepared an updated State Health Plan that will provide the basis for a comprehensive health status report in 2005. |
Coordinate supportive social services. A variety of social services can help vulnerable populations gain timely access to the health care system and complement health care as well. One of the most important support services is transportation. People who cannot get to a physician's office or health center, for example, will surely not be well-served by the system. Many lower-income people have no car and must rely on public transportation to keep their medical appointments. Some take two or three buses to do this. In some cases, however, transportation is simply not attainable. Thus, the city should develop ways to improve public transportation through enhanced bus service, van pools, taxi rides, etc.
Nutrition services can also be an effective complement to good medical care, since working-age adults, children, and senior citizens who are poorly nourished will frequently suffer adverse health consequences.
Substance abuse treatment services are also critically important. Some health plans place strict limits on covered services for substance abuse, while uninsured people may face long queues for this type of care. This can result in avoidable and expensive trips to the emergency room.
Another key area involves language barriers. The District has a sizeable population of people who either do not yet know English or are struggling to learn it. It is vitally important to have linguistically and culturally sensitive physicians, nurses, and allied medical personnel. Practitioners who can speak to these residents in their native language are frequently in short supply. Translators can provide an important second line of support. These steps can help the District address the health care needs of the immigrant population, who are estimated to account for about 9,000 of the uninsured. Finally, it is important to establish and enforce "safe havens" for undocumented members of the city to obtain care without fear of investigations or reprisals.
Maximize public health dollars. The District should improve its ability to purchase health care for Medicaid beneficiaries and the uninsured based on full accountability of health plans and providers for cost and quality under DOH's oversight. Given that most Medicaid beneficiaries will be enrolled in Medicaid HMOs, the District has an opportunity and obligation to assure that it is a prudent purchaser of high-quality services from the PBC, District hospitals, and other providers. The District government should make the transition, in stages if necessary, from its current approach to a system where dollars follow patients and where providers and health plans are more accountable for patient outcomes. Safety-net providers will need to make their case (to the District and to patients) that they can meet the District's requirements at a reasonable cost and with good health outcomes.
Improve the effectiveness of the Public Benefit Corporation. The District should work with the PBC management and PBC board to immediately undertake an independent comprehensive assessment. The findings from this assessment should provide the basis for redefining the PBC's structure and functions within the District's overall safety-net system. The new purchasing method would incorporate service quality and health outcome measures.
In June 2000 the District Council adopted the final resolution containing the Commission's recommendations. This report details the analytical bases for the Commission's recommendations and presents strategies for achieving these goals. Unity of purpose between the executive and legislative branches will continue to be an essential element for achieving real change. As with earlier analyses, the challenge is now in our ability to turn words into actions.
Crucial next steps involve the development and implementation of detailed operational plans and budget estimates for proposals in the final resolution. Success will depend on leadership provided by elected officials, health care providers, and health advocates, especially those focusing on the health care safety net. Collaboration among these constituencies is critical; it was the premise behind the composition of the Commission and the spirit of its final recommendations.
In consultation with the community, the Mayor's office will develop these plans and convey budget proposals to the Council.
Long-term evaluation of health care reform in the District will focus on health statistics and other indicators of residents' well-being. Intermediate indicators will include expanded access to primary care, increased numbers of insured residents, and enhanced integration and information-sharing among health care institutions. Most importantly, at a time of economic expansion and newfound fiscal responsibility, measures of success must be assessed by our progress in meeting the health needs of those who previously had inadequate access to services, particularly the indigent and uninsured.
The windfall from the tobacco settlement may provide limited funds for some health care initiatives. Other enhancements will come from existing resources and system efficiencies. More than finances, however, success will come from all parties, public and private, working together to accomplish true health care reform. The Commission's resolution is a road map that builds upon past successes and challenges the District to forge new alliances in getting the job done.
CON - Certificate of Need
DCHF - DC Healthy Families
DCPCA - DC Primary Care Association
DCQHCs - District of Columbia Qualified Health Centers
DOH - Department of Health
DSH - Disproportionate Share Hospital
FEHBP - Federal Employees Health Benefits Program
FPL - Federal Poverty Level
FQHCs - Federally Qualified Health Centers
HCFA - Health Care Financing Administration
HPSAs - Health Professional Shortage Areas
LISC - Local Initiatives Support Corporation
MIS - Management Information Systems
MUAs - Medically Underserved Areas
PBC - Public Benefit Corporation
PCPs - Primary Care Physicians
PDPA - Pharmaceutical Drug Payment Assistance program
QI - Quality Improvement
SCHIP - State Children's Health Insurance Program
SHPDA - State Health Planning and Development Agency
TANF - Temporary Assistance for Needy Families
TITLE XIII. HEALTH CARE SYSTEM DEVELOPMENT COMMISSION
Sec. 1301. Short title.
This title may be cited as the "Health Care System Development Commission Establishment Emergency Act of 1999".
Sec. 1302. Establishment; purpose.
There is established a Health Care System Development Commission ("Commission") to develop recommendations and an implementation plan for developing the health care system.
Sec. 1303. Qualifications; membership; terms of office.
(a) The Commission shall consist of 11 members as follows:
(1) There shall be 3 ex-officio voting members as follows:
(A) The Mayor of the District of Columbia ("Mayor");
(B) The Chairman of the Council of the District of Columbia ("Council"); and
(C) The Chairman of the Council's Committee on Human Services.
(2) There shall be 5 members appointed by the Mayor and 3 members appointed by the Council by resolution.
(A) Appointed members of the Commission shall be persons with proven expertise in health care delivery, finance, insurance, public health, integrated health care delivery systems, or strategic planning.
(B) Appointed members of the Commission shall be residents of the District.
(b) A vacancy on the Commission shall be filled in the same manner that the original appointment was made.
(c) The Commission shall select a chair from among its ex-officio members.
(d) Six members of the Commission shall constitute a quorum.
(e) The term of members shall end 180 days after the effective date of this act.
Sec. 1304. Compensation.
Members of the Commission shall not receive compensation or reimbursement for actual expenses incurred in the performance of official duties.
Sec. 1305. Duties.
(a) The Commission shall establish criteria to be used in the development of recommendations. The criteria shall include, but not be limited to, the following:
(1) Efficiency and effectiveness of the District's health care system;
(2) Access to quality health care services;
(3) Consistency with financial plan and budget of the District;
(4) Community impact; and
(5) Economic benefits.
(b) Within 120 days after its initial meeting, the Commission shall develop a set of recommendations for developing the health care system which addresses the following:
(1) Inpatient bed over-capacity;
(2) Distribution of health care services and providers;
(3) The role and the needs of the District of Columbia Public Benefit Corporation;
(4) Maintenance of safety net providers;
(5) Impediments to accessing care beyond the lack of health care insurance;
(6) Fiscal impact of expanding health insurance coverage, including a study of the utilization of available health maintenance organization coverage by the Medicaid eligible population for each year since the advent of Medicaid HMO coverage in the District of Columbia, and the number of medically indigent District residents who have been provided care at area hospitals as compared to the total number of medically indigent persons who have received care in each hospital in each of the past 3 years;
(7) Implementation schedule for developing the health care system; and
(8) Other issues.
(c) The recommendations shall be developed in accordance with the criteria established in this section.
Sec. 1306. Approval of recommendations.
(a) The Mayor shall transmit the recommendations of the Commission to the Council for approval.
(b) The recommendations shall be transmitted to the Council for a 45-day period, excluding days of Council recess. The Council shall take action to approve or disapprove the recommendations. If the Council does not take action within the 45-day period, the recommendations shall be deemed disapproved.
Sec. 1307. Office space and staffing.
(a) The Mayor shall provide sufficient office space, detail staff, and technical and administrative support to assist the Commission in the fulfillment of its duties.
(b) The Commission shall have the authority to request directly from each department, agency, or instrumentality of the District government, and each department, agency, or instrumentality is hereby authorized to furnish directly to the Commission upon its request, any information deemed necessary by the Commission to carry out its functions under this act.
Sec. 1308. Fiscal impact statement.
This title will have no fiscal impact because Commission members are unpaid and existing resources will support the Commission's activities.
13-594
A RESOLUTION IN THE COUNCIL OF THE DISTRICT OF COLUMBIA
June 26 2000
To approve, on an emergency basis, the recommendations of the Health Care System Development Commission.
RESOLVED, BY THE COUNCIL OF THE DISTRICT OF COLUMBIA, That this resolution may be cited as the "Health Care System Development Commission Recommendations Emergency Approval Resolution of 2000".
Sec. 2. Pursuant to section 1306 of the Health Care System Development Commission Establishment Act of 1999, effective October 20, 1999 (D.C. Law 13-38; to be codified at D.C. Code § 6-155) ("Act"), the Mayor transmitted to the Council for approval the following recommendations of the Health Care System Development Commission to develop the District's health care system:
Recommendations:
(1) Improve the health care delivery system and services for vulnerable populations by:
(A) Establishing a certification program that designates local health centers (and planned centers) as DC Qualified Health Centers ("DCQHC"). This program will be guided by the state health plan, the certificate of need ("CON") program, and community input. The certification would include practice standards and reporting requirements and would ensure that the centers are part of an integrated, comprehensive system of health care providers that includes hospitals, laboratories, pharmacies, and other health services and their patients would have increased access to needed secondary and tertiary care. The certification process will include community input.
(B) Using new Disproportionate Share Hospital ("DSH") dollars, consistent with federal standards, to increase the accessibility of local medical homes that provide preventative and primary care to all District residents. Hospitals receiving DSH payments will be held responsible for increasing the availability of outpatient and primary care services, for formalizing relationships with local health centers (including hospital health centers) that lead to greater patient access to secondary and tertiary care, and for reporting to the Department of Health ("DOW) the number of patients serviced and services provided with the hospitals' DSH dollars.
(C) Activating provisions of existing laws that enable the District to contract with the Public Benefits Corporation to provide hospital-based and clinic-based health services for the uninsured. This contract would use cost-effective reimbursement methodologies for in-patient services as well as comparable methodologies for outpatient and clinical services. Service quality and outcome measures will be incorporated in the contract. A comprehensive assessment, overseen jointly by the District and the PBC, will be conducted. The results of that assessment will provide the basis for refining/reviewing the PBC's structure and function within the District's health care safety net.
(D) Establishing a public/private capital fund that will help build the capacity of the District's community-based delivery system. Because the District has a public trust, District funds would be available initially to public clinics and public/private partnerships. Every effort would be made to establish funding to meet the needs of public and, private health centers and hospital clinics that are DCQHCs or have DOH-approved plans for becoming DCQHCs. The health centers receiving capital funds will be approved under the CON process based on DOH's determination that their improvement or construction helps meet state plan-identified needs. These centers will also receive technical assistance. The capital fund will be developed using District capital funds that will be matched by the private sector.
(E) Providing a higher Medicaid reimbursement rate for community health centers certified as DCQHCs or with DOH-approved plans to become DCQHCs. This will allow the District to provide additional funding to those centers that serve large percentages of uninsured individuals and centers that provide care in areas of the District where too few primary care providers operate.
(F) Developing a pharmaceutical program that continues the existing program for the uninsured when it expires in 2002. The program will work through participating pharmacies to provide free or discounted prescription drugs to uninsured residents.
(2) Expand Health Insurance Coverage by:
(A) Expanding DC Healthy Families coverage to adults without dependent children in phases once enrollment increases have been achieved and experiences assessed from the current implementation. Phase I will cover adults with incomes up to 50% of the federal poverty level (FPL); Phase II will cover adults with incomes up to 100% FPL.
(B) Providing tax credits to businesses offering health coverage to District residents, subject to actuarial estimates.
(C) Establishing a "brand" insurance coverage program which could include Medicaid beneficiaries and D.C. government employees and could be open to small businesses. A "brand" insurance card will be issued to all participating individuals and will include a code to distinguish among benefit plans. The ultimate goal is to create a "seamless system care.
(D) Proposing a change in the Federal Employee Health Benefit Program to permit the inclusion of District of Columbia small businesses and District government employees. This would require Congressional legislation.
(3) Build the capacity of the Department of Health to ensure the public's health and better manage the health system by:
(A) Increasing enrollment in DC Healthy Families (DCHF) through:
(i) Implementation of an electronic (web-based) enrollment system, improved training, and outreach efforts to register Medicaid eligible and uninsured patients at hospitals and DCQHCs and to provide a greater level of accountability.
(ii) Maximization of TANF and SCRIP funds earmarked for enrollment.
(iii) Implementation of presumptive eligibility for all children.
(iv) Implementation of a 1-year continuous enrollment program for all, including parents of DCHF and future DCHF expansion populations, including adults without dependent children.
(B) Developing the Department of Health's monitoring-and management capacity through:
(i) Development of a state-of-the-art, outcomes measures-based, MIS system that links DOH to health care providers throughout the District and the provision needed staff development training to implement this system.
(ii) Rewriting the District's State Health Plan and Medicaid State Plan.
(iii) Restructuring the Certificate of Need process and the reassessment, and rewriting if appropriate, of regulatory and reporting requirements.
(4) Goals to be accomplished include to:
(A) Improve the health care system and services for vulnerable populations.
(B) Increase insurance coverage and decrease the number of uninsured District residents.
(C) Improve the capacity of the Department of Health to monitor and assess the quality and effectiveness of the health system.
Sec. 3. Pursuant to section 1306(b) of the Act, the Council approves the recommendations of the Commission.
Sec. 4. Fiscal impact statement.
Health Care System Development Commission recommendations are subject to enabling legislation, regulation, and appropriations. Therefore, there is no fiscal impact.
Sec. 5. The Secretary to the Council shall transmit a copy of this resolution to the Mayor upon its adoption.
Sec. 6. This resolution shall take effect immediately.
| Total Uninsured | 100% | ||
| Age | |||
| Children under age 19 | 24.3% | ||
| Adults 19-64 | 74.5% | ||
| Adults 65+ | 1.2% | ||
| Sex | |||
| Male | 55.2% | ||
| Female | 44.8% | ||
| Race | |||
| White | 23.7% | ||
| Black | 71.9% | ||
| Other | 4.4% | ||
| Income as % of Poverty | |||
| <100% FPL | 27.5% | ||
| 100-200% FPL | 35.5% | ||
| 100-133% | 11.9% | ||
| 133-150% | 9.1% | ||
| 150-200% | 14.3% | ||
| >200% FPL | 37.2% | ||
| Family Income | |||
| <$20,000 Family Income | 50.0% | ||
| $20,000-$39,999 | 28. | 28.7% | |
| >$40,000 | 21.7% | ||
| Total Uninsured Adults (over 18) | 100% | ||
| Age | |||
| 19-24 | 16.7% | ||
| 25-34 | 34.8% | ||
| 35-44 | 26.8% | ||
| 45-54 | 13.2% | ||
| 55-64 | 6.9% | ||
| 65+ | 1.6% | ||
| Sex | |||
| Male | 56.1% | ||
| Female | 43.9% | ||
| Race | |||
| White | 24.5% | ||
| Black | 70.6% | ||
| Other | 4.9% | ||
| Income as % of Poverty | |||
| <100% FPL | 29.0% | ||
| 100-200% FPF | 34.0% | ||
| 100-133% | 10.3% | ||
| 133-150% | 7.4% | ||
| 150-200% | 16.3% | ||
| >200% FPL | 37.0% | ||
| Family Income | |||
| <$20,000 Family Income | 54.7% | ||
| $20,000-$39,999 | 27.1% | ||
| >$40,000 | 18.2% | ||
| Total Uninsured Children (under 18) | 100% | ||
| Age | |||
| <age 6 | 36.3% | ||
| 6-14 | 50.1% | ||
| 15-18 | 13.7% | ||
| Sex | |||
| Male | 52.3% | ||
| Female | 47.7% | ||
| Race | |||
| White | 21.2% | ||
| Black | 75.8% | ||
| Other | 3.0% | ||
| Income as % of Poverty | |||
| <100% FPL | 22.7% | ||
| 100-200% FPL | 39.3% | ||
| 100-133% | 17.0% | ||
| 133-150% | 14.4% | ||
| 150-200% | 7.9% | ||
| >200% FPL | 38.0% | ||
| Family Income | |||
| <$20,000 Family Income | 33.8% | ||
| $20,000-$39,999 | 33.7% | ||
| >$40,000 | 32.4% | ||
Note: This table does not include potential savings from increased efficiencies at the PBC or at the CMHS, nor does it include potential additional sources of funds such as supplemental Medicaid payments, certification of public expenditures, savings generated from enrolling the remaining fee-for-service Medicaid beneficiaries in managed care, or increases in DC's DSH allotment.
| Source of Funding | Amount | Notes/Sources | |
| District Resources | |||
| DC General direct subsidy | $28,4750,000 | FY98 from PBC audited financials; $1,464,801 of which is the DC share of DSH payment to DC General | |
| PBC clinics direct subsidy | $17,900,000 | FY98 from PBC audited financials | |
| PBC indirect subsidy (e.g., in-kind services, loan forgiveness) | $ | ||
| District share of Medicaid expendituresD-a | $317,338,972 | FY98 HCFA 64 reports | |
| Subsidy to St. Elizabeth's for DC share of DSH payment | $829,934 | Lewin 3/99 report; MAA FY99 | |
| DC share of DSH payments to private hospitals | $7,562,408 | Lewin 3/99 report; MAA FY99 | |
| DC share of DSH correction | $692,000 | DOH FY2000 Proposed Budget | |
| Commission on Mental Health Services (CMHS) | $123,750,000 | DOH FY 2000 Proposed Budget (District's recommendations) | |
| Addiction Prevention and Recovery Administration (APRA) | $25,355,000 | DOH FY2000 Proposed Budget | |
| Public Health Service (includes MCH, Nutrition, School Health, etc.) | $9,409,000 | DOH FY2000 Proposed Budget | |
| Preventive Health Services (includes STDs, TB, Chronic Disease, Injury, etc.) | $4,649,000 | DOH FY2000 Proposed Budget | |
| Agency for HIV/AIDS | $7,976,000 | DOH FY2000 Proposed Budget | |
| Environmental Health Administration (includes Lead Poisoning) | $8,090,000 | DOH FY2000 Proposed Budget | |
| Subtotal District | $555,884,314 | ||
| HCFA-Medicaid | |||
| Federal share of Medicaid expendituresD-b | $556,554,356 | FY98 HCFA 64 reports | |
| Federal share of DSH payments | $23,000,000 | FY98 HCFA 64 reports | |
| Federal share of DSH correction | $9,000,000 | Lewis 3/99 report | |
| District's allotment of TANF/Medicaid Delinking Fund | $3,259,072 | From a total of $500 million in federal matching funds at enhanced rates (90% for the first $2 million used for qualified outreach activities. Thereafter, 90% match for "beneficiary-oriented activities"; 75% for other allowable activities). | |
| Subtotal Medicaid | $591,813,428 | ||
| Other sources of Federal Funds | |||
| Grants to APRA | $4,173,000 | DOH FY2000 Proposed Budget | |
| Funding for CMHS | $62,312,000 | DOH FY2000 Proposed Budget (District's recommendations) | |
| Public Health Service | $23,636,000 | DOH FY2000 Proposed Budget | |
| Preventive Health Services | $6,900,000 | DOH FY2000 Proposed Budget | |
| Agency for HIV/AIDS (includes Ryan White CARE Act) | $42,725,000 | DOH FY2000 Proposed Budget | |
| Environmental Health Administration | $9,021,000 | DOH FY2000 Proposed Budget | |
| Subtotal Other Sources of Federal Funds | $148,767,000 | ||
| Tobacco Settlement Money | |||
| Tobacco settlement allocation (initial payment December 1998) | $14,570,839 | Starting in 2000 and ending in 2025, total annual payments range between $32.9 million and $50.9 million. The District's total settlement through 2025 of $1.3 billion of the total $205 billion settlement.D-c | |
| Tobacco settlement allocation (initial payment January 2000) | $15,007,964 | ||
| Tobacco settlement allocation (annual payment April 200) | $23,918,943 | ||
| Subtotal Tobacco Settlement | $53,497,745 | ||
| TOTAL | $1,349,962,488 | ||
D-a. Includes Medical Assistance Payments (MAP), excluding DSH,
and administrative costs.
D-b. Includes Medical Assistance Payments (MAP), excluding DSH, and administrative costs.
D-c. The District has not yet determined how to spend its tobacco settlement allocation.
Tobacco settlement money is not federal funds; it is a transfer from tobacco companies.
The District currently spends little or no funds on tobacco prevention.
Source: State Health Planning and Development Agency.
| Life Stage | Indicator | District of Columbia | United States |
| Prenatal | Percent of women receiving first trimester prenatal care, 1997 | 56 | 82 |
| Birth | Low birth weight: percent of live births, 1997 | 13.5 | 7.5 |
| Infant mortality rate per 1,000 live births, 1997 | 13.1 | 7.1 | |
| Children | Percent of children age 19-35 months who received full vaccination series (4DPT/3 polio/MMR), 1998 | 84 | 78 |
| Young adults | Incidence of gonorrhea per 100,000, 1997 | 882 | 123 |
| Incidence of syphilis per 100,000, 1997 | 21 | 3.2 | |
| Incidence of AIDS per 100,000,1996 | 230 | 27.8 | |
| Older Adults | Tuberculosis cases per 100,000, 1996 | 25.6 | 7.7 |
| Age-adjusted cancer mortality per 100,000, 1996 | 196 | 128 | |
| Age-adjusted mortality due to heart disease, per 100,000,1996 | 179.1 | 105 | |
| Diabetes as a contributing factor to death, per 100,000, 1995 | 90 | 41 | |
| Pneumonia and influenza mortality, per 100,000, 1996 | 22.1 | 17.3 |
Sources: District of Columbia data from D.C. Department of Health, District of Columbia Healthy Resident Year 2000 Plan, Progress Review 1993-1998, June 8, 1999. Cardiovascular data courtesy of Dr. Joy Phillips, D.C. Center for Health Statistics. United States data from National Center for Health Statistics, Healthy People 2000 Review 1998-1999, Hyattsville, MD, Public Health Service, 1999.
As shown in the Figure below, the distribution of the District's DSH payments to private hospitals does not correspond closely to the distribution of care of the uninsured. DC General Hospital admits about one-third of the total number of charity patients. Another third of the uninsured go to DSH hospitals, and a third to non-DSH hospitals.
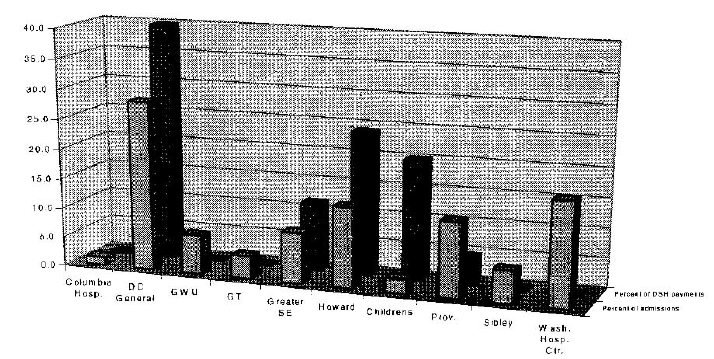
| Columbia Hosp. | DC General | GWU | GT | Greater SE | Howard | Children's | Providence | Sibley | Wash. Hosp.Cent. | |
| Admissions | 1.3% | 28.4% | 6.6% | 3.8% | 8.5% | 13.6% | 2.4% | 12.6% | 5.5% | 17.4% |
| DSH payments | 0.0% | 39.8% | 0.0% | 0.0% | 11.5% | 24.1% | 20.1% | 4.6% | 0.0% | 0.0% |
Source: Schamess A et al. "A Profile of the Health Care Delivery System and the Health Status of District Residents." An unpublished report prepared for the Health Care Systems Development Commission, October 26, 1999.
G-a. More recent data from 1997 are available, but are incomplete. However, the partial 1997 data appear to reflect the same disparities between the allocation of DSH funds and the burden of charity care distributed among the District's hospitals.
A set of standards should be established that all health centers that wish to receive money from the public-private partnership or directly from the District must meet. These standards would define "safety net providers" and thus identify where public support should be targeted. Thus, the District of Columbia should establish a process to certify (by the Department of Health or a comparable agency) that safety-net providers meet criteria to become D.C. Qualified Health Centers. The following criteria have been suggested by the District of Columbia Primary Care Association, but the Commission recommends that there be community input prior to the adoption and implementation of these standards:
The Washington, D.C., office is one of 42 program sites of the Local Initiatives Support Corporation, a national nonprofit intermediary that channels private sector financial and technical resources to community development corporations (CDCs). LISC's mission is to assist CDCs in transforming distressed neighborhoods into healthy communities. LISC serves as a lender, advocate, funder, broker, and technical assistance provider. The primary focus is to build the organizational and technical capacity of CDCs so that they can effectively sponsor and develop physical and social development projects that benefit their communities.
Headquartered in New York City, LISC is governed by a 25-member Board of Trustees and managed by a central operations staff that provides financial, legal, management, and information services and support to the staff located in 42 sites. LISC has three affiliates: National Equity Fund (NEF), Local Initiatives Managed Assets Corporation (LIMAC), and The Retail Initiative (TRI).
Established in 1982, the Washington, D.C., LISC program is operated by a director with four program officers and two administrative assistants. Local staff operate with the guidance of a Local Advisory Committee, composed of program funders and other resources people.
Source: From materials produced by the Washington, D.C., LISC office at 1825 K Street, NW, Suite 1100, Washington, DC 20006.
Prepared for the Health Care Systems Development Commission by Powell, Goldstein, Frazer & Murphy, LLP.
The purpose of this memorandum is to discuss the District of Columbia's options for creating an enhanced outpatient payment program for private and public primary care providers to improve quality, stability, coordination, and capacity in the District's primary care system. This memorandum presents considerations for provider eligibility, financing, funding limitations, and preliminary cost estimates.
It is possible to structure increased Medicaid payments to certain providers, both public and private. Eligible providers could be limited to-those who are the only providers located in certain wards of the city, serve high numbers of uninsured or Medicaid patients, provide unique or specialized services, or for providers in need of additional payments to adjust to managed care. If a system of certifying non-profit and PBC primary care centers as "District of Columbia Qualified Health Centers (DCQHCs)" is established in the future, eligibility for any enhanced outpatient payment program could be tied to certification as a DCQHC.
Preliminary reports of the subcommittees have identified the need to create better access to primary care by the uninsured by stabilizing and expanding the current infrastructure, and expanding enrollment and eligibility for Medicaid and SCHIP. An enhanced primary care and outpatient program could help to finance the stabilization and expansion of primary care services while supporting needed outreach to increase enrollment under an expansion.
Outpatient program enhancements could include payments to providers to help offset losses related to care of Medicaid and indigent patients. Program enhancements could also include access to capital to support modernization of existing facilities and development of new primary care and urgent care centers. The program could support the District's investment into the creation of a comprehensive, cost-effective pharmacy management and subsidy program and increased enrollment outreach as the population of Medicaid eligible is expanded.
The cost estimates below represent the full costs (state and federal share) of each of a number of possible short-term initiatives. As a general matter, these initiatives could be implemented by the District with, at most, a state plan amendment. It is suggested that all of the proposals of both subcommittees (coverage and facilities) be clustered into short and longer-term initiatives, with the latter to be financed through a §1115 demonstration.
Medicaid is an obvious source of financing for many parts of these enhanced outpatient and primary care initiatives. Financing the 30 percent state share could be accomplished through direct appropriation of District money or through certification of public expenditures, intergovernmental transfer, or provider tax. Certification offers the District the opportunity to gain federal matching funds based on money that is already being expended through its public providers. Likely sources of CPE are unreimbursed costs for services provided by the PBC, St. Elizabeth's Hospital, and MRDDA, and the otherwise unreimbursed costs for substance abuse treatment and school health services. (See additional memorandum describing CPE in more detail.) In most cases, these unreimbursed costs must be associated with Medicaid recipients, although in the DSH context and under a §1115 demonstration, they may be associated with the uninsured as long as they represent costs which Medicaid will pay.
The opportunity to gain federal match is limited by the District's $32 million Medicaid DSH annual spending limit and the relevant Medicare-related upper payment limits.
DSH: So long as DC Medical Assistance Administration (MAA) plans to allocate the entire Medicaid DSH amount, there is no room to increase Medicaid DSH spending without a reallocation of existing spending.
Upper payment limits (UPLs): The best information available is based on an analysis performed by consultant Diane Plumb for DC MAA in 1996. As the District proceeds with planning for Medicaid program enhancements, a follow-up should be performed to test the assumptions of the 1996 analysis. As discussed in previous analyses, the UPLs for the District (based on the 1996 analysis) are:
In sum, we believe that an updated analysis should be performed that perhaps challenges some of the previous conservative UPL calculations. In the meantime, however, previous analyses indicated that an estimated $5.6 to $17 million could be dedicated to funding an enhanced outpatient program. The District would have to provide the state match (30 percent) to draw down the necessary funds, but if this could be accomplished using certified public expenditures or intergovernmental transfers, the District's need to allocate fewer new funds to provide the state match would be reduced.
We strongly recommend that certain aspects of the recommendations of both Subcommittees should be incorporated into an expanded §1115 demonstration. If the District obtains HCFA approval of a Medicaid §1115 demonstration, there is a budget neutrality requirement that extends though the term of the waiver. The District should prepare for future §1115 waiver applications by projecting savings attributable to enhancing the infrastructure for primary care delivery and reducing unnecessary emergency room and inpatient hospital utilization.
Sources and methods of capital financing should be examined carefully for the capital portion of the enhanced outpatient program. The Facilities Subcommittee has suggested a "primary care community development" program using a local non-health organization experienced in this type of funding. Other public systems have utilized a number of capital funding options, including:
Finally, tobacco settlement funds are a large source of potential future financing for an enhanced outpatient program. Additional sources might also include the assets of conversion foundations created by the sale of not-for-profit health care institutions in the District (e.g., GW and Greater Southeast). Nationally, state legislators have considered restrictive mandates over how the assets of these foundations are to be used, and District lawmakers may want to consider targeting these funds to assist in capital and other assistance for safety-net primary care providers.
J-a States have the flexibility to set rates based on a provider's percentage of indigent patients. However, states cannot make Medicaid payments to providers for services to those who are not Medicaid eligible without a §1115 waiver.
Medicaid
SCHIP
All children under age 19 (not already categorically eligible for Medicaid or covered by employer-sponsored health insurance) under 200% of FPL [BBA 1997]
Non-Waiver Medicaid Expansions
Waiver Expansion (§ 1115 waiver submitted to HCFA on October 29, 1999 is pending approval)
K-a. The District's medically needy standard is about 50 percent of the federal poverty level (FPL), which is equal to about 121 percent of the AFDC payment standard.
Estimates of the number of individuals who would be eligible for the expansion program were developed using pooled 1995 and 1996 Current Population Survey (CPS) demographic data on the District (adjusted to correct for problems with the data). These figures were adjusted to reflect other population control totals where available. The Lewin Group's State Medicaid Eligibility Model (SMEM) was then used to estimate the number of individuals who meet age, residency, and income eligibility criteria for the proposed expansion program. In determining the number of individuals who would enroll in the program, participation or takeup rates for the expansion population were developed based on the average national Medicaid participation rate (76 percent) and the overall District Medicaid participation rate (86.6 percent). Separate rates were developed for those who already have employer-sponsored health coverage (40 percent) and those who do not already have employer-sponsored coverage (84 percent). For adults without dependent children, the District reduced the participation rates by 20 percent to reflect expected difficulties in reaching these individuals through outreach.
In general, cost estimates are based upon per capita monthly Medicaid costs for similar persons already covered under the program, where possible. Costs for newly eligible categories that are not now covered are based upon the current HMO premium rates for the AFDC and AFDC-related population that are adjusted to reflect age differences in cost based on actuarial data. Total program costs are equal to the estimated average monthly per member costs for each eligibility category multiplied by the estimate of the monthly number of persons that would enroll in the program. Historical growth rates in per-capita costs by eligibility group are considered in making assumptions about the total cost of the program over the waiver period. Assumed annual growth rates equal the lesser of the estimated average rate of growth in District spending by eligibility group (here, AFDC adults) from 1993-1997 and the national average historical rate of growth for these eligibility groups. In this case, the District's average rate of growth of 2.40 percent, rather than the national growth rate of 5.51 percent, was used. Projected costs are periodically adjusted to reflect the actual costs of serving the expansion group. If program costs are overestimated costs, the Federal government makes the difference available to the District in DSH funds. If program costs are underestimated, the District pays back the difference to the Federal government.
L-a. All of the enrollment and cost estimates included in this proposed expansion program and in both §1115 waivers that were submitted to HCFA were prepared by the Lewin Group using 1995 and 1996 CPS data on the District and available District Medicaid data.
Federal spending for a state's waiver expansion program cannot exceed what federal spending would have been on a state's Medicaid program in the absence of the expansion program. The cost of a waiver program to the federal government must be fully offset by a corresponding reduction in federal spending under some other parts) of the Medicaid program.
The budget neutrality requirement applies for any Medicaid waiver program, such as for a waiver that changes the eligibility criteria for Medicaid. For example, the District wants to expand Medicaid eligibility to a group of individuals who are not categorically eligible for Medicaid (adults without dependent children). There are several mandatory categories of individuals to which states must extend Medicaid eligibility if they operate a Medicaid program. There are also several optional categories of individuals to which states can extend Medicaid eligibility. For these categorically eligible groups (both mandatory and optional), the state receives federal Medicaid matching funds to pay for the cost of serving the groups. In the District, the federal matching rate is 70 percent for all Medicaid groups and 79 percent for SCHIP-eligible kids. It is important to note that for a state to draw down any federal Medicaid matching funds, it must show HCFA that it has funds available to subsidize its share of the program's costs.
States must include in their waiver proposal to the Health Care Financing Administration (HCFA) a "paper analysis" of how they intend to meet budget neutrality requirements. Using five years of Medicaid historical data of member per month costs (taking into account a growth factor for the waiver period equal to the lesser of state-specific growth rates and national growth rates), states must determine costs for the base year (which is the year just prior to the demonstration program's start year). States must show HCFA: (1) what it costs currently for its Medicaid program; and (2) the expected growth rate for the program. States must show that the proposed program will be budget neutral to the federal government over the entire waiver period. HCFA has a Budget Neutrality team, which includes HCFA staff and staff from the Office of Management and Budget (OMB), which reviews the waiver's budget neutrality provision and guides and works with the state to get the data it needs to show budget neutrality. The budget neutrality process is an evolving process that lasts throughout the demonstration/waiver period. Budget neutrality is monitored through state submission of the HCFA-64 Medicaid and Disproportionate Share Hospital (DSH) quarterly expenditure reports. These reports separate DSH expenditures and demonstration expenditures (which are now considered Medical Assistance Payments [MAP] and not DSH).
M-a. This information was obtained from conversations with staff at the Health Care Financing Administration (HCFA), as well as from the HCFA Web site, 1999.
Prepared for the Health Care Systems Development Commission by the Economic and Social Research Institute
Challenge: There are more than 80,000 uninsured residents in the District. While some of these individuals are eligible for Medicaid or SCHIP, but not enrolled, other uninsured residents with very low incomes are not eligible for public programs and do not have access to employer-sponsored health insurance. The largest group of low income individuals who are ineligible for public programs today are adults without dependent children.
Initiative: The District would expand Medicaid eligibility to all adults without dependent children below 100 percent of poverty.
Likely Impact: The initiative would make approximately 26,000 adults without dependent children eligible for Medicaid; it is estimated that just over 15,000 adults will actually enroll. Of these, roughly 14,000 individuals would otherwise have been uninsured. Therefore, this initiative could have a direct impact on reducing the number of uninsured District residents.
Cost: The average cost of the program per year would be $41.8 million (combined federal and District costs) and the total cost of the program over a five-year demonstration period would be roughly $200 million (combined federal and District costs). The federal share of the cost of the program must be budget neutral to the federal government. The District would be responsible for financing $12.5 million per year and $61.4 million over the five-year period.
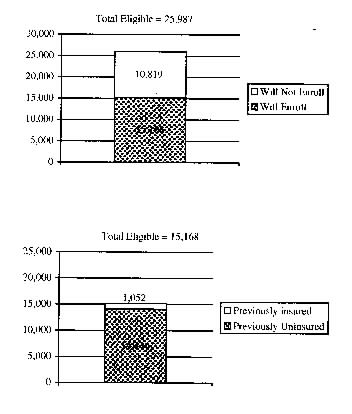
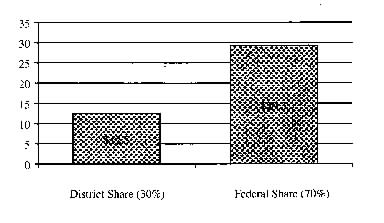
N-a. According to the U.S. Census Bureau, the federal poverty
level (FPL) in 1998 was $13,003 for a family of three and $16,660 for a family of four.
N-b. See Appendix L for details on how these enrollment estimates
were derived.
N-c. See Appendix L for details on how these enrollment estimates
were derived.
Prepared by the Government of the District of Columbia, Department of Health, Medical Assistance Administration
| Number Actually Enrolled | Number Expected to EnrollO-b | Percentage of Expected Enrollment | Universe of Eligible People | Percentage of Universe Enrolled | |
| Expansion Children (SCHIP and insured) | 2,782 | 5,601 | 50% | 8,957 | 31% |
| Eligible but not Enrolled Children | 3,727O-c | 4,023 | 93% | 10,579 | 35% |
| Parents of all Eligible Children | 5,871 | 6.714 | 87% | 6,714 | 87% |
| Total | 12,380 | 16,338 | 76% | 26,250 | 47% |
O-a. DC Health Families includes all children
eligible for Medicaid or SCHIP and all parents of eligible children.
O-b. Based on take-up rates associated with other expansions.
O-c. As of November 1999.
District of Columbia Health and Hospitals Public Benefit Corporation. "Health Care in the District of Columbia: Prescriptions for Change." Prepared by John A. Fairman and submitted to Eugene Kinlow, March 15, 1999.
District of Columbia Health and Hospitals Public Benefit Corporation. "Health Care Systems Development in the District of Columbia and the PBC: A Databook." December 1999.
District of Columbia Health and Hospitals Public Benefit Corporation. "The Heart of the Safety Net." Slide Presentation to the District of Columbia Health Care Systems Development Commission, December 8, 1999.
District of Columbia Health and Hospitals Public Benefit Corporation. "Reforming Health Care in the District of Columbia: Tailoring Change to Real-Life Citizen Needs." April 14, 1999.
District of Columbia Hospital Association. "Annual Report." DCHA, 1998.
District of Columbia Hospital Association. "Financial Indicators, Fiscal Year 1997." DCHA, Fall/Winter, 1998.
District of Columbia Hospital Association. "Utilization Indicators, Calendar Year 1998." DCHA, Spring, 1999.
District of Columbia Primary Care Association. "Primary Health Care Services for the Medically Needy in the District of Columbia: A 1997 Update." November 1997. (NOTE: This paper is in the process of being updated by the DCPCA.)
District of Columbia Primary Care Association. "Stable and Capable: The Future of the District's Primary Care Safety Net."
Health Care Now. "How the Community Sees Health Care in the District of Columbia: The Barriers to Getting Needed Care Go Well Beyond Not Having Insurance." Center for Community Change.
Kaye PE. "A Brief Overview of the Organization and Funding of Health Services in the District of Columbia." Working Draft prepared for the Center for Community Change, D.C. Community Health Advocacy Initiative and distributed at the D.C. Consumer Health Summit, June 19, 1999.
The Lewin Group, Inc. "A Plan to Expand Coverage under Medicaid in the District of Columbia." Prepared for the Department of Health, Medical Assistance Administration, March 17, 1999.
Medical Assistance Administration, Department of Health. "District of Columbia Medicaid Program: 1998 Annual Report."
Non-Profit Clinic Consortium Position Paper. "Health Reform in the District of Columbia, 1999: The Need for Primary Health Care for the Uninsured." May 10, 1999.
Ormond BA and RR Bovbjerg. "The Changing Hospital Sector in Washington, D.C.: Implications for the Poor," The Urban Institute, October 1998.
Ormond B et al. "Health Care for Low-Income People in the District of Columbia," The Urban Institute, May 1999.
Sherry ST. "D.C. Health Status Data." Working Draft prepared for the D.C. Community Health Advocacy Initiative and distributed at the D.C. Consumer Health Summit, June 19, 1999.
Sherry ST. "Opportunities for Community Organizing in D.C. Health Laws and Regulations." Working Draft prepared for the D.C. Community Health Advocacy Initiative and distributed at the D.C. Consumer Health Summit, June 19, 1999.
Rosenbaum S et al. "Assessing the Ambulatory Health Care Needs of Low Income Uninsured D.C. Residents in a Changing Health Care System." February 1999. (Study commissioned by the Non-Profit Clinic Consortium.)
Rosenbaum S et al. "Primary Care in the District of Columbia: What are the Needs of Uninsured Patients Served at Community Clinics (Findings from a Survey of Community Health Providers)." April 25, 1999. (Study commissioned by the Non-Profit Clinic Consortium.)
United States General Accounting Office. "District of Columbia: Information on Health Care Costs." GAO/AIMD-96-42, April 1996.
Walker B. "The Burden of Chronic Disease in the District of Columbia." Prepared for the Mayor's Health Policy Council, May 11, 1999.
Carpenter MB and L Kavanagh. "Outreach to Children: Moving from Enrollment to Ensuring Access." Arlington, Virginia: National Center for Education in Maternal and Child Health, 1998.
Center for Budget and Policy Priorities. "Free and Low-Cost Health Insurance: Children You Know are Missing Out (An Outreach Kit)."
CHIP Working Group. "CHIP Communications Handbook." Courtesy of Wyeth-Lederle Vaccines.
Coughlin TA and D Liska. "The Medicaid Disproportionate Share Hospital Payment Program: Background and Issues." The Urban Institute, Series A, No. A-14, October 1997.
Ladenheim K. "Patching the Safety Net, Part II." National Conference of State Legislatures, January 1999.
Pulos V and LG Lynch. "Outreach Strategies in the State Children's Health Insurance Program." June 1998 (www.familiesusa.org/OUT2.HTM)
United States General Accounting Office. "Health Care Access: Opportunities to Target Programs and Improve Accountability." Statement of Bernice Steinhardt. GAO/T-HEHS-97204.
District of Columbia Office of the Chief Financial Officer (www.dccfo.com)
District of Columbia Department of Health (www.dchealth.com)
- including Medical Assistance Administration (MAA), Primary Care Office, State Health
Planning and Development Agency (SHPDA)
District of Columbia Hospital Association (DCHA) (www.dcha.org)
District of Columbia Primary Care Association (DCPCA) (www.dcpca.org)
Health Care Financing Administration (www.hcfa.gov)
Health Resources and Services Administration (www.hrsa.-gov/profiles/d.c/)
Local Initiatives Support Corporation (www.liscnet.org)
Non-Profit Clinic Consortium (www.npcclinics.org)
The Urban Institute (www.urban.org)
Mayor Anthony A. Williams, Commission Chair
Mayor Anthony A. Williams has served as Mayor of the District of Columbia since
January 2, 1999. Prior to this, he was the District's Chief Financial Officer from October
1995 to June 1998. During his tenure as CFO, Mr. Williams succeeded in reforming the
District's floundering financial system and guiding the city budget to a surplus of $185
million in fiscal year 1997. Before coming to District government, he was appointed by
President Clinton as CFO for the U.S. Department of Agriculture. Mr. Williams also served
as the Deputy State Comptroller for the State of Connecticut.
Linda W. Cropp, Chair, Council of the District of Columbia
Linda W. Cropp has served as chair of the Council of the District of Columbia
since 1997 and as an At-Large member of the Council since 1990. Previously, Chair Cropp
served as president and vice president of the District's Board of Education. Mrs. Cropp
began her 27-year career in public service as a school teacher and guidance counselor.
Earlier, as Chair of the Committee on Human Services, Mrs. Cropp oversaw the creation of
the DC DOH.
Sandra Allen, Chair, Committee on Human Services
Sandra Allen is the Ward 8 representative to the Council of the District of Columbia.
Councilmember Allen has dedicated 17 years of her professional life in service to the
government of the District of Columbia. Ms. Allen served 12 years as a District Advisory
Neighborhood Commissioner and has worked to improve community organizations and the
services they provide.
Marsha Lillie-Blanton, Dr.P.H.
Marsha Lillie-Blanton is a vice president of The Henry J. Kaiser Family Foundation, where
she directs the Foundation's policy research and grant making on access to care for
vulnerable populations on which she has written numerous studies. She is also an assistant
professor of health policy at Johns Hopkins University. Dr. Lillie-Blanton has more than
15 years of experience in health policy research and management. She previously served as
associate director of the Kaiser Commission on Medicaid and the Uninsured.
Martis James Davis
Martis "Marty" Davis is managing director of Burson-Marsteller's Washington
office. Through his broad experience, Mr. Davis has gained a clear understanding of
marketing communications, business and labor management, crisis mitigation, and the role
communications can play in enhancing the delivery of health services and in addressing
barriers to health access. He currently is also on the board of the Public Benefit
Corporation.
Larry S. Gage
Larry S. Gage is president of the National Association of Public Hospitals and Health
Systems, as well as a partner at Powell, Goldstein, Frazier & Murphy, LLP. Mr. Gage is
a recognized leader in the development of national, state, and local policies affecting
urban hospitals and health systems and the patients they serve. Health issue areas in
which he has authored studies and developed strategies include: Medicare and Medicaid
reimbursement, health professions education, AIDS, emergency and trauma care, and drug
abuse prevention.
Gilbert Hahn, Jr.
Gilbert Hahn, Jr., senior partner of Amram and Hahn, gained prominence in Washington,
D.C., as chairman of the Council of the District of Columbia, serving in this capacity
from 1969 to 1972. Throughout his long career as an attorney and businessman, Mr. Hahn has
served on the boards of numerous District organizations and health providers, including
serving as president of the Washington Hospital Center and chairman of the DC General
Hospital Commission.
Sister Carol Keehan
Sister Carol Keehan has served as president and chief executive officer of Providence
Hospital Center since 1989. She also currently serves as chair of the DC Hospital
Association. With degrees in both nursing and business management, Sister Carol has more
than three decades of experience in the operation of non-profit hospitals and the delivery
of health services to low-income and vulnerable populations. She has also served on the
boards of numerous civic organizations and health providers and has frequently advised
government leaders on health care access issues.
Andrew Schamess, M.D.
Dr. Andrew Schamess is currently Senior Deputy Director for Primary Care at the District
of Columbia Department of Health. Previously, he was the medical director of La Clinica
del Pueblo, a health center serving a largely Hispanic population located in the Mount
Pleasant area of the city. Dr. Schamess is also an assistant clinical professor of health
care sciences and internal medicine at Howard University and chair of the DC Nonprofit
Clinic Consortium. Additionally, he is the author of several articles on providing health
care to underserved populations.
Loretta Tate
Loretta Tate is currently the acting president and chief executive officer of the Marshall
Heights Community Development Organization and on the board of the Public Benefit
Corporation. Ms. Tate has 17 years of experience in the fields of law enforcement and
human services. Her major priorities in these areas have focused on increasing access to
health care, expanding substance abuse treatment and prevention services in Ward 7, and on
improving the safety and welfare of urban communities.
Henry J. Werronen
Henry Werronen is president of Werronen Company, Inc., a health care consulting firm
specializing in strategic planning, integrated health care delivery systems, managed care,
and Medicaid. Prior to founding his consulting firm, he spent 10 years with Humana in
Louisville, Kentucky, and was the founder and chief operating officer of the Humana Health
Plan. Mr. Werronen provides technical assistance and design services to health systems
within the District and across the United States.
Staff Director - Diane C. Lewis
Diane C. Lewis is the executive vice president for ALTA Consulting Group, Inc., a
management consulting firm that advises health care delivery systems and assists community
development/revitalization efforts in underserved areas of the District. Ms. Lewis has
also created marketing strategies to aid community-based health networks in successfully
competing or contracting with managed care organizations and behavioral health networks.
Government of the DISTRICT OF COLUMBIA
Additional Copies .available:
On the Internet:
http://www.washingtondc.gov/
By Mail :
Office of Policy and Evaluation, Executive Office of the Mayor
441 4th Street, Northwest
Room 920 South
Washington, DC 20001
By Telephone:
202-727-6979
1. AARP, Reforming the Health Care System: State Profiles 1997, Washington, DC: Public Policy Institute, 1997.
2. These numbers are based on the experience of Los Angeles County. The Los Angeles County Department of Health Services (LA DHS), under a HCFA §1115 Demonstration waiver, has fundamentally restructured their County health care delivery system. In so doing, they have tried to address some of the same concerns currently confronting the District, such as the need to reduce inappropriate inpatient care and expand outpatient care. LA DHS has outlined some of their achievements in the most recent waiver extension application to HCFA. For example, they report that inappropriate use of the emergency room has decreased by 27 percent since the demonstration began. In addition, they have decreased the number of budgeted inpatient beds by 28 percent, decreased the average inpatient daily census by 24 percent, and reduced the average length of stay from 6.4 days to 5.9 days. Source: Medicaid Demonstration Project for Los Angeles County §1115 Waiver Extension Proposal Fiscal Years 2000-2005.
3. Source: Kaiser/HRET, October 1999.
![]()
Send mail with questions or comments to webmaster@dcwatch.com
Web site copyright ©DCWatch (ISSN 1546-4296)